A three-judge panel of the U.S. 5th Circuit Court of Appeals ruled the state’s requirement that abortion clinics meet ambulatory surgical center standards — which include minimum sizes for rooms and doorways, pipelines for anesthesia and other infrastructure — did not impose an undue burden on a “large fraction” of Texas women seeking abortions.
Only a handful of Texas abortion clinics — all in major metropolitan areas — meet those standards, which are costly to implement. Immediately following the ruling, the Center for Reproductive Rights and Texas women’s health care providers announced their plan to appeal the case to the U.S. Supreme Court.
“Once again, women across the state of Texas face the near total elimination of safe and legal options for ending a pregnancy, and the denial of their constitutional rights,” said Nancy Northup, president and CEO of the Center for Reproductive Rights, which brought the lawsuit after the passage of the 2013 law.
In the lawsuit, the Center for Reproductive Rights, on behalf of several Texas abortion providers, also asked the court for a reprieve for two clinics from a separate provision of the law that requires doctors who perform abortions to have admitting privileges at a hospital within 30 miles of an abortion clinic.
One of those clinics, Reproductive Services in El Paso, has since closed. In ruling against exempting the El Paso clinic, the judges found that women in the area did not face a “substantial obstacle” in obtaining an abortion because they could travel to New Mexico for the procedure.
The judges ruled in the provider’s favor in regard to Whole Women’s Health in McAllen, granting an exemption to the hospital admitting privileges rule and to some narrow elements of the ambulatory surgical center requirements. Since the McAllen clinic stopped performing abortions in late 2013 — and after the closure of a Corpus Christi clinic — women in the Rio Grande Valley must travel more than 200 miles to get an abortion, which the judges said was too far.
But they left in a big caveat: The McAllen clinic is exempt only until there’s another Texas abortion clinic closer to the Rio Grande Valley than San Antonio — anywhere within 150 miles.
Amy Miller, the CEO of Whole Women’s Health, said Tuesday that it remains unclear whether the McAllen clinic will be able to remain open.
Texas Attorney General celebrated Tuesday’s ruling, saying the court had validated the state’s “authority to establish safe, common-sense standards of care.”
“HB 2 both protects the unborn and ensures Texas women are not subjected to unsafe and unhealthy conditions,” he said.
But the legal fight is likely to continue. Abortion providers could request that the full 15-member court hear the case, or they could attempt to take the matter to the U.S. Supreme Court. The 5th Circuit is considered one of the nation’s most conservative federal appellate courts.
NARAL Pro-Choice Texas Executive Director Heather Busby decried the ruling as a “travesty” that would leave open only eight clinics statewide.
“The 5th Circuit has once again put their political ideology above the law and failed to recognize that HB 2 is an undue burden on Texans’ access to safe, legal and timely abortion,” she said. “Your zip code should not determine your health care.”
Reporter Liz Crampton contributed to this story.
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/public-health/tough-texas-abortion-restrictions-upheld-by-appeals-court/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=546722&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>It’s a regimen Riley says she wouldn’t have started if it weren’t for the medical team at Memorial Health System of East Texas. Unable to afford a mammogram after discovering the lump, Riley, 47, received a free cancer screening at the system’s Livingston facility, a private specialty clinic that participates in the joint state-federal Breast and Cervical Cancer Services program. Doctors there helped her enroll in Medicaid to cover costs related to treating her cancer, including a double mastectomy performed two weeks ago.
“It saved my life,” Riley said of the cancer screening program. The disease “would’ve killed me within the year.”
Riley fears future women might not be so lucky.
The conservative Texas Senate, in its running effort to put Planned Parenthood clinics out of business, is considering changing how funding is distributed through the cancer screening program for poor, uninsured women.
Under the chamber’s proposed plan, public entities like state, county and community health clinics would get first crack at the cash. “Non-public entities” that provide screenings as part of “comprehensive” primary and preventive care would come in second place.
And private specialty clinics like the Livingston facility would only get cancer-screening funding if there’s money left over. That includes Planned Parenthood — whose family planning and cancer-screening clinics are a target of GOP lawmakers even though they are prohibited from performing abortions if they receive tax dollars.
The Senate’s chief budget writer, state Sen. Jane Nelson, R-Flower Mound, has said the proposed tiered funding is intended to ensure that facilities unaffiliated with abortion providers are funded first.
But under the proposed funding revisions, at least 34 providers not affiliated with Planned Parenthood — nearly one-fifth of those currently using program dollars — would be moved into the second or third tier for funding.
“There’s not going to be anything left by the time it gets to us,” said Carol Belver, executive director of Community Action Inc. of Central Texas, whose three clinics screened a combined 625 women in the San Marcos area last year. Though her clinics provide primary care, the cancer screenings are offered as a separate service — leaving Community Action in the bottom tier for funding.
“We’re the collateral damage,” she added.
The screening program, which is primarily funded with federal dollars, served 33,599 Texas women in fiscal year 2014 — 57 percent of whom were Hispanic.
In some rural parts of the state, the funding change could leave the sole program provider in the area with little to no funding for cancer screenings. In Amarillo, for example, four Haven Health clinics are the only program providers, but they would all likely fall into the third tier for funding.
Patricia Jones, director of community-based care for Memorial Health System of East Texas, which treated Riley, said Memorial is the only program contractor with clinics in Livingston, Lufkin and San Augustine.
“We’ve had this funding almost 20 years, and if we were to lose that funding, you have 350 ladies who lose this access to a complex system,” Jones said. “You’d have 20 cancers that wouldn’t have been diagnosed as early as they were.”
In Abilene, Amy Fulcher, the women’s health case manager at the Abilene Diagnostic Women’s Health Clinic, said that if her organization lost program funding, poor women seeking cancer screenings through the program would have to travel at least 150 miles in any direction. Her clinic is the only provider in town.
“This whole situation is very frustrating because it started as a target against Planned Parenthood,” Fulcher said.
For years, the Republican-led Legislature has worked to keep Planned Parenthood and other organizations even loosely affiliated with abortion providers from receiving state dollars for health care for poor women. In 2011, lawmakers ousted the organization from the joint state-federal Medicaid Women’s Health Program, leading the federal government to withdraw its match. It’s unclear whether the feds will take similar action this year if the Legislature approves the changes to the cancer-screening program.
For now, Planned Parenthood clinics continue to receive funding from the cancer-screening program, serving 10 percent of the women who participate in the program.
Democrats have accused Republicans of playing politics with women’s access to life-saving procedures, and are promising to put up a fight.
“The approach is problematic, if for no other reason [than] it’s not making decisions based upon health care — it’s making decisions for women’s health based on politics,” said state Sen. Kirk Watson, D-Austin.
Asked about the negative effect the funding changes could have on clinics that aren’t affiliated with Planned Parenthood, Nelson said she was looking into it.
“I am still investigating this issue to ensure we proceed in a way that preserves access to services for women,” she said in a statement.
For now, the future of the program remains unclear. That leaves Riley, the cancer patient, to worry about the fate of other women in Texas who cannot afford cancer screenings.
“It’s very scary for the women that are going to come up after me that aren’t going to be able to get the help they need,” Riley said.
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/in-texas-funding-fight-cancer-care-for-poor-women-could-be-collateral-damage/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=527024&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Rose Okoro, a nurse practitioner who specializes in family medicine, opened the  in Katy, Texas, last October. Seven months later, she has only enough patients to work there part time.
It is not because of demand but because of a law that ties the work of nurse practitioners to doctors, said Okoro, who has a doctorate in nursing practice. State regulations do not allow her to be reimbursed by insurance companies unless the physician who supervises her has a contract with those companies.
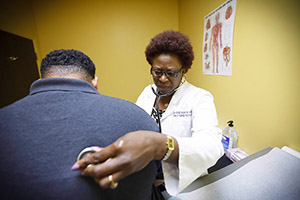
Dr. Rose Okoro is a nurse practitioner who owns Daystar Family Clinic in Katy, Texas. She says she has struggled to treat a greater number of Medicaid patients because of state regulations (Photo by Michael Stravato/Texas Tribune).
“Any approval the collaborating physician does not have, I cannot get — even if I’m qualified,” said Okoro, who has worked as a nurse practitioner for five years and as a registered nurse for 10 years before that. “It’s so frustrating for us to open a clinic and then we’re not able to see everybody.”
Nurse practitioners in Texas have Ěý˛ą˛µ˛ąľ±˛Ô˛őłŮĚý that link them financially and professionally to supervising physicians, a construct they say ties their hands and limits their ability to treat patients in a state with a looming shortage of primary care physicians. Texas lawmakers  during the last legislative session following a compromise with physician groups, which argue that nurse practitioners do not have the training or experience to be entirely independent. But nurse practitioners are still battling for increased autonomy in the state Medicaid program.
Texas offers health coverage to poor children and people with disabilities through a managed care system in which private insurance companies contract with the state to enroll patients and cover medical services like doctor visits and prescriptions. Nurse practitioners argue that  passed by lawmakers last year should have allowed them to be approved by these state-contracted insurance companies even if their supervising physicians did not treat patients on Medicaid — a growing trend given the low reimbursement rates. But state officials and the physician lobby said that interpretation of the bill was never agreed upon.
“Obviously we have found out that not everyone is in agreement with the language in the bill and what it accomplishes,” said Kathy Hutto, a consultant for the . The coalition and another advocacy group, , helped negotiate the terms of the bill.
Stephanie Goodman, a spokeswoman for the state’s , which oversees Medicaid in Texas, said the bill is “silent on the issue” of whether nurse practitioners could treat Medicaid patients whose insurers had not signed on with the supervising physicians.
“There was a work group put together on the bill in the session, and members of that work group have different memories as to what happened or any decisions that were made,” Goodman said. She added that insurers who participate in the state’s Medicaid program oppose changes to the contractual requirement that the supervising physicians be approved in order for the nurse practitioners to be approved.
Michael Hazel, president of Texas Nurse Practitioners, said the current discord “is just another example of one profession creating unnecessary barriers” for another.
Physicians say the issue is about patient safety, not about creating barriers. They point to the four years of medical school and three years of residency training that primary care physicians must complete after obtaining an undergraduate degree. Nurse practitioners, meanwhile, must complete four years of nursing school and usually two additional years in a graduate-level training program, either through a master’s or doctoral program.
Doctors also say the current “team-based” model — in which doctors who have more comprehensive training partner with nurse practitioners who offer clinic-based treatment — is effective.
The powerful physician advocacy groups involved in the negotiations on last session’s bill, including the , which represents more than 47,000 physicians and medical students, and the , say the Medicaid issue was tabled after an agreement was not reached.
“Any suggestion that we agreed to it is, frankly, a revision to history,” said Dan Finch, director of the medical association’s legislative affairs division. “Having said that, we understand their concerns, and we’re trying to address that.”
After a series of meetings last week, the physician groups have come back to the negotiating table with alternatives to the exemption that nurse practitioners want. The potential solutions offered by the physicians would give nurse practitioners more flexibility when it comes to Medicaid health plans but are designed to maintain the current supervisory relationship.
The nurse practitioners said they were willing to compromise on a temporary fix in order to not delay care for patients, and were waiting for the commission to determine which solution would be adopted. But they insisted that this would serve only as a “patch,” and planned to readdress the issue during the next legislative session. Â
Beyond issues with Medicaid, they are ultimately pushing for complete independence from doctors as part of a national effort.
They have been successful in several states, including Arizona, Colorado and New Mexico. In Texas, nurse practitioners argue that barriers to their practice of medicine, like the Medicaid requirement, prevent the state from effectively responding to growing primary care needs, particularly in underserved rural communities.
With the next legislative session eight months away — and a growing number of doctors no longer accepting Medicaid patients because of low reimbursement rates and the red tape of filing claims — nurse practitioners are hoping for a fix soon.
“I’m certainly hopeful that we can come up with a solution that allows care to be provided during this interim,” said Hutto, the consultant to the nurse practitioners coalition. “And then if we need to clean up the language next session we can do that.”
Disclosure: The Texas Medical Association is a corporate sponsor of The Texas Tribune. Texas Nurse Practitioners was a corporate sponsor of the Tribune in 2012.Â
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/texas-nurse-practitioners-scope-of-practice-supervision/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33677&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
LAREDO — For 12 hours a day, the waiting room at Dr. Gustavo Villarreal’s family practice is often packed with patients, people who will pay a flat $50 fee for the convenience — or necessity — of a walk-in, quick-turn doctor’s visit. Villarreal’s practice, which does not accept any form of health insurance, has thrived despite its location in a city where nearly one-third of the population lives below the federal poverty line.
At both the state and federal level, efforts are underway to decrease Texas’ sky-high rate of residents without health coverage. But Villarreal is among a rising number of primary care practitioners who have given up on the red tape of filing insurance claims, switching to a cash-based model that is growing in popularity among Texas’ insured and uninsured patients.
Doctors who use this model, which they call “direct primary care,” say they can keep their costs competitive by avoiding the bureaucracy of the health insurance system and the high processing costs — including additional staff — associated with accepting coverage.
“It had always been affordable and possible to maintain a practice with what insurance and patients paid, but about 10 or 15 years ago, you started seeing a decline” in revenue, said Villarreal, who switched his traditional family practice to its current business model in 2012.
Most doctors limit their services to basic or preventive care — treatment their patients can afford without turning to their insurance providers — such as prescribing medicine for colds and infections, treating minor lesions and overseeing long-term care for conditions like diabetes and osteoporosis.
When patients need additional treatment for serious ailments or tests and procedures that cannot be done in-house — MRIs and X-rays, for example — physicians working under the direct primary care model refer patients to specialists and technicians who accept insurance.
While many of his patients are uninsured, Villarreal, who has been practicing medicine for more than three decades, said he also regularly treats patients who have health insurance but are trying to avoid shelling out thousands of dollars to meet high deductibles.
Some health care experts worry that if too many practitioners choose this path, the state could be left struggling to find doctors to accommodate patients with insurance at a time when federal health care reform is making such coverage mandatory for most Texans. So far, efforts to enroll Texans in the federal insurance marketplace — crucial to the success of the Affordable Care Act — have made a small dent in the state’s uninsured population, which has reached 6 million people, according to United States census data. The U.S. Department of Health and Human Services reported that as of March 1, 295,000 Texans had signed up for insurance coverage in the federal marketplace.
“We have to find ways of stretching the current number of primary care doctors to meet that demand,” said Dr. Clare Hawkins, president of the Texas Academy of Family Physicians. “Direct primary care goes in the other direction.”
Insurers say consumers should have flexibility when it comes to their health services, but they warn that not having health insurance leaves individuals unprotected from the hefty price tags associated with unanticipated medical costs.Â
“Consumers should anticipate their medical needs,” said David Gonzales, executive director of the Texas Association of Health Plans. “However, when that is not possible, consumers should have financial protection from the unexpected.”
The direct primary care model is not new. Before Congress passed legislation in 1973 that led to the through pre-paid health plans, or health maintenance organizations, physicians largely operated through this fee-for-service medical model. And the percentage of doctors who have reverted to this approach in Texas in recent years is not huge: 10 percent of Texas physicians do not currently have contracts with health insurers, according to preliminary results from a 2014 Texas Medical Association survey.
Lee Spangler, vice president of medical economics with the TMA, said Texas is seeing an increase in practices like these because they give doctors more flexibility to determine the services they provide and to cut costs for their practices.
“A physician has very little ability to negotiate all policies and procedures that come with insurance contracts,” Spangler said, adding that some insurance companies can even dictate the business hours during which doctors can be paid. “Basically you get rid of all those shackles in terms of having a carrier dictate to the practice how to deliver medical services.”
But it is the business model that proves most attractive to physicians, Spangler said, adding that doctors “want to get out from under what has been stacked up on them.”
Under the current health insurance system, physicians who treat covered individuals submit claims for the services they provide and receive reimbursements to cover their costs. Private insurance providers and government-subsidized health programs like Medicare and Medicaid each have their own rules and regulations for filing claims, including specific timeframes and billing systems.
Health providers who treat poor children and people with disabilities also face heightened scrutiny from state and federal agencies charged with , leaving that they could be subject to unwarranted or costly investigations.
Doctors who have embraced the direct primary care model have done it with a wide range of approaches. And most tout that the costs they’ve cut by forgoing insurance give them the ability to scale back on the number of patients they must see each day to turn a profit.
In Austin, Drs. William and Mason Jones — a father-son team — practice “concierge medicine,” treating patients under a membership model in which patients pay annual fees for access to a variety of services, including unlimited office visits, routine vaccinations and round-the-clock medical assistance by phone.
Mason Jones said his office is a “low-volume practice” that gives him the “luxury of time” to spend with patients. “This works out great for preventive medicine,” he said.
In Corpus Christi, Dr. Coleen Madigan said she only works two days a week, during which she visits with about five patients a day and is able to make house calls. She said this gives her the opportunity to spend as much time with her patients as they require.
In Laredo, Villarreal has had the opposite experience. His business model frees up time for him to see even more patients, he said, without the additional costs to his practice that come from filing insurance claims. He continues to see 40 to 60 patients a day, he said, 20 of whom tend to be new to his practice.
“To me, there’s no other way I would practice medicine,” he said. “You feel like you’re a doctor again.”
Disclosure: The Texas Medical Association and the Texas Association of Health Plans are corporate sponsors of The Texas Tribune. A complete list of Texas Tribune donors and sponsors can be viewed .
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/texas-trib-doctors-turn-to-cash/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32873&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>