How many nurses does it take to run a hospital?
Legislatures in at least seven states and the District of Columbia are trying to answer that question as they debate bills that would require hospitals to have a minimum number of nurses on staff at all times.
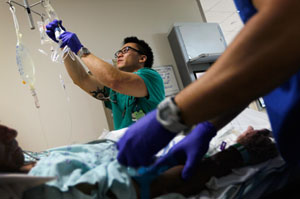
Registered Nurse Tung Tran hangs an I.V. bag for a patient at the University of Miami Hospital’s Emergency Department in 2012 in Miami. California is the only state that has a minimum nurse staffing law, but at least seven other states are considering adopting their own versions (Photo by Joe Raedle/Getty Images).
So far, only one state has such a law. California’s state legislature passed a in 1999. Since then, similar nurse staffing laws have failed in every other state where they were proposed. But the nursing unions backing the bills have grown increasingly powerful in statehouses across the country.
Hospital administrators are vehemently opposed. They argue the bills would strip them of their ability to make basic staffing decisions and be a financial burden. Many nurses and nursing unions say legislation is needed to prevent cost-conscious hospitals from endangering patients by putting too large of a workload on too few nurses.
“Hospitals right now are run like businesses and they’re focused on the short-term bottom line,” said Jeff Breslin, president of the Michigan Nurses Association, a union backing in the Michigan legislature. If the bill becomes law, he said, “it doesn’t matter what part of the state you’re in, you can be assured you’re going to have adequate nursing care whatever place you’re going into.”
Lawmakers in , , , , , and are also considering legislation. While the language differs across the states, at the heart of all these bills is a minimum nurse-to-patient ratio — a fixed number of nurses per patient.
The bills call for a different ratio in different parts of a hospital. For example, the proposed law in Michigan would require hospitals to maintain a one-to-one ratio — no less than one nurse for every patient — in all operating rooms across the state. In pediatric units, that ratio can go as high as one nurse for every four patients.Ìý
A 2004 of research conducted by the U.S. Agency for Healthcare Research and Quality found that patients at hospitals with low nurse-to-patient ratios fare worse than those at hospitals with higher ratios. But nursing and hospital advocates say there is scant research on what the ideal ratios should be, and there are about whether mandating a ratio by law ultimately improves patients’ health, according to hospital and nurses’ groups.
“We’re trying to create a standard where hospitals will be required to have adequate staffing levels,” said Dawn Kettinger, a spokesperson with the MNA. “It would be great if hospitals did this on their own, but unfortunately they’re not doing that.”
Joyce Young, a nursing administrator with St. Joseph Mercy Health System in the Detroit area, said many hospitals are, in fact, creating minimum staffing levels on their own, especially now that they’re penalized for certain negative patient outcomes under the federal health law.
“Hospital nursing leaders are in positions such that they can be able to determine staffing levels,” Young said. It shouldn’t be “based upon a legislator who mandates a number. It should be left to the nurses.”
The California Experiment
Today, only California requires all of its hospitals to maintain a minimum nurse-to-patient ratio. If a hospital sees a surge of patients due to something unexpected, like a car crash or an outbreak, it still must meet the minimum ratio. The only time a hospital can go under the minimum ratio is during what the statute calls a “healthcare emergency.”
Jolee Cochran, a registered oncology nurse who has been working at Cedars-Sinai Medical Center in Los Angeles for 26 years, said the law has made her job more manageable. Before, she said, it wasn’t uncommon for a nurse to be responsible for seven patients at a time. Now, it would be a violation of the law for her to have more than five patients under her care.
Cochran said patients in her hospital are much sicker than they used to be and require much more complex care. “I can’t imagine having more than five patients with one nurse, with the type of patients we have now,” she said.
But she also said the law has made scheduling shifts more challenging. Because the staffing ratios in California apply at all times, if a nurse goes on a break, “there has to be someone there to cover you,” Cochran said. “By law, you can’t fudge that or else you get fined.”
Jan Emerson-Shea, vice president of the California Hospital Association, agreed with Cochran that the law’s rigidity – its “at all times” clause – is a major problem for health providers in the Golden State. She also said the ratios written into the law in California were merely a political compromise that had no basis in scientific evidence.
However, Emerson-Shea said hospitals in her state have slowly learned to live with the law.Ìý
“We don’t fight this issue now,” Emerson-Shea said. “It’s the law of the state. … It’s over. It’s done.”
Victory, Then Defeats
What was a major victory for nurses in the Golden State 14 years ago has been followed by a string of defeats elsewhere. “Hospitals go to holy war to prevent it,” said Chuck Idelson, a spokesman for National Nurses United, a 185,000-member labor union founded four years ago in California.
NNU is the primary backer of the staffing ratio bills currently working their way through various state capitols. However, not all nurses back the union’s legislative push.
The American Nurses Association, a professional trade group that advocates on behalf of both unionized and non-unionized nurses, opposes staffing ratio bills. Janet Haebler, the association’s director of state government affairs, said she doesn’t expect any others will pass this year.Ìý
Haebler said understaffing is a major problem, but that calcifying a nurse-to-patient ratio into law isn’t the right way to solve it. The association instead favors laws that require hospitals to set up committees made up of nurses and administrators that work together to create staffing plans.
“We’re respectful of all approaches as long as nurses have input,” she said. “In California, there’s no input. It’s just … ‘This is what it will be at all times.'”
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/nurse-staffing-laws/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=24737&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>Nursing unions say the proposed Patient Protection Act codifies into law minimum staffing levels that are needed to maintain patient safety, while hospitals say the cost of hiring new nurses to comply with the law would put them out of business.
The ratios called for in the bill vary depending on the hospital department. In a pediatrics unit, the bill would require no less than a 1-to-4 nurse-to-patient ratio. In the operating room, hospitals would have to maintain a 1-to-1 ratio — one nurse for every patient at all times.
Deidre Beckford, a nurse at MedStar Washington Hospital Center who has worked there for more than 20 years, says understaffing has forced her to take care of five to six patients at a time.
“There are times when I have to do the dressing on patients and I can’t get to it,” she said. “I have to put antibiotics on patients and they’re late. You have to turn patients every two hours and you can’t get to it. It infringes on their care.”
Washington Hospital Center didn’t respond to Beckford’s claims about infringed patient care, but its chief nursing executive, Sue Eckert, said in an email to KHN that the hospital manages its staffing levels collaboratively with nurses and that those levels can fluctuate depending on how many patients it has and how sick those patients are.
The nursing bill in D.C. would reduce some of this fluctuation. It’s modeled after a nearly identical law that took effect in 2004 in California, the only state to require minimum staffing ratios in its hospitals. So far, it’s unclear whether this requirement has had a positive or negative effect in California hospitals.
Studies have shown that the law has led toÌý in California and a decrease in nurse turnover due to burnout. But researchers also found thatÌý on some hospitals.
When it comes to the ultimate question of whether this law reduced patient mortality, , a nursing professor at the University of Nevada, Reno, who has examined the effects of the California law, says the .
“That’s the big question everyone wants an answer to,” she said.
Citing positive outcomes of the California law, the labor union National Nurses United is strongly pushing for the staffing ratio bill in D.C., which has been assigned to a committee but has no scheduled hearings as of yet. Nine of the Council’s 13 members signed on as co-introducers last week.
But the District of Columbia Hospital Association is waging an all-out campaign against it, supporting aÌý that contains many of the same provisions as the Patient Protection Act but without the staffing ratio mandate. Robert Malson, the association’s president, says his organization is also scheduling individual meetings with every council member to try to persuade some of them to change their minds.
Malson said he’s been informing them of “exactly which hospitals would go out of business, and in which sequence” if the Patient Protection Act passes, though he wouldn’t share that information with KHN.
He said the bill is an attempt to get legislators involved in D.C. hospitals’ labor negotiations with its nurses, which have been far from harmonious in recent years. Almost two years ago, nurses at Washington Hospital CenterÌý a few months after voting overwhelmingly to join NNU, the largest nursing union in the country.
Serratt says the dueling bills are a sign that the relationship between hospitals and nurses in D.C. has grown dysfunctional.
“If you have really strong communication and good people on both sides of the table, we wouldn’t have the government getting in the middle of this kind of stuff,” she said.
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/dc-hospitals-nurses-staffing-ratios-fight/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=25422&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in collaboration with
A magazine ad for the testosterone drug AndroGel shows a discount card that allows consumers to pay “as little as $10 per month” for the medicine. Drugmaker GlaxoSmithKline announces in another magazine that it offers discount coupons for the popular inhaler Advair. And a TV commercial for Nexium notes that if consumers can’t afford the heartburn drug, its manufacturer, AstraZeneca, “may be able to help.”

In the past few years, coupons and discount cards have become nearly ubiquitous for prescription drugs. Such incentives are available for 395 medications, according to from industry consultant IMS Health. In in 2009, a marketing firm found that only 86 drugs came with coupons.
Drugmakers say the coupons help Americans get the medicine they need. But the insurance industry is concerned that they drive patients toward more expensive brand-name drugs, leaving insurers to cover the full cost, which then gets passed on to consumers in the form of higher premiums.
“An individual patient who receives a coupon might not realize that, although that particular prescription may cost less that month, overall what it does is to raise costs for everyone, including themselves,” said Susan Pisano, a spokeswoman for the industry trade group America’s Health Insurance Plans.
For people using Medicare, Medicaid, veterans benefits or any other federal health insurance program, using a coupon or a discount card to buy prescription medication works against efforts to keep federal spending down and may also be counter to federal law, according to some experts’ interpretation.
Coupon Wars
Prescription drug coupons represent the latest battle in an escalating war between health insurers and the pharmaceutical industry.
Insurers set high co-pays for brand-name drugs to steer their members to less-expensive generics. In response, companies such as Merck, AstraZeneca, Pfizer and many others issue coupons or discount cards that cover that co-pay.
outlined the dramatic effect coupons can have on prices paid by consumers. Using cholesterol-lowering drugs as an example, researchers found that the popular statin Lipitor comes with an average co-pay of $30 a month, compared with a $10-a-month co-pay for simvastatin, a generic drug also used to treat high cholesterol. But with a coupon from Pfizer, the drug’s manufacturer, the co-pay for Lipitor goes down to $4 a month, making it less expensive for the consumer than simvastatin.
It’s a great deal for the patient, but not the insurer. According to the JAMA article, the insurer pays $18 a month for simvastatin and $137 a month for Lipitor.
The coupons are “designed to get patients to bang down their doctor’s door and say, ‘Give me the most expensive drug,’ ” said Mark Merritt, president of the Pharmaceutical Care Management Association. Merritt’s trade group represents companies that manage prescription benefit plans for private insurance companies and firms that participate in Part D, Medicare’s drug program.
Merritt said that, since insurers ultimately end up footing the bill for the more expensive brand-name drug, they may respond by increasing premiums on everyone.
The rising cost of brand-name drugs is one of the many factors driving up the cost of health care. President Barack Obama addressed the issue at a White House news conference in 2009 during the debate over his health-care bill. When asked if Americans would have to make sacrifices to make the overhaul work, he said, “They’re going to have to give up paying for things that don’t make them healthier. . . . If there’s a blue pill and a red pill, and the blue pill is half the price of the red pill and works just as well, why not pay half price for the thing that’s going to make you well?”
Drugmakers argue the coupons save money by preventing health problems that occur when patients cannot afford prescribed medications. in JAMA found that 20 percent of Medicare beneficiaries in fair to poor health did not take their medicine as directed because of cost concerns.
“By reducing patient cost sharing, co-pay coupons can support patients’ adherence to a treatment regimen,” Matthew Bennett, vice president of the trade group PhRMA, said in a statement. “[They] can play a valuable role in generating better health outcomes and reducing the use of avoidable and costly medical care.”
The coupon war is now being fought in state legislatures and in court. Earlier this year, several union health plans filed a class-action lawsuit against drug manufacturers over coupons. They’re asking a judge to find the use of coupons illegal and for monetary damages. In July, prescription coupons. It had been the only state to ban them.
Illegal Kickbacks?
The cost issue surrounding coupons is made even more complicated when the federal government is the insurer.
According to federal statutes, it is a crime to provide “any remuneration to induce or reward referrals reimbursable by a federal health care program.” Some experts say coupons constitute such remuneration because they encourage consumers to purchase a more expensive product, with the extra cost ultimately falling on taxpayers. from the Congressional Budget Office found that Medicare pays an additional $76 every time a senior chooses a brand-name drug over a generic.
Even officials within the pharmaceutical and insurance industries said coupons should not be used by beneficiaries of government health programs. “The use of co-pay coupons is prohibited in the Medicare Part D program and pharmacies,” Bennett said, “and coupon-processing vendors have safeguards in place to prevent unauthorized use.”
But others say the coupons’ status is not resolved.
According to Donald White, a spokesman for the Department of Health and Human Services, no court or administrative body has ever ruled that coupons are illegal. HHS has never prosecuted anyone for issuing or using coupons in the federal health programs.
— commissioned by the National Coalition on Health Care this spring — found that 6 percent of Medicare beneficiaries are using the coupons.
“I can’t blame a senior” for doing so, said Larry McNeely, manager of policy communications at the coalition, which is comprised of unions, businesses and others seeking to reduce health-care spending and expand coverage to the uninsured. “[But] these aren’t put out there for anyone’s health. They’re there to cripple competition from generics.”
Moral Hazard
Merritt said prescription drug coupons create a moral hazard for all parties involved.
“No one has an incentive to do the right thing,” he said. “The doctor has no incentive to not give out coupons to seniors. If the pharmacist says no, it will be pretty easy for a senior to go to the next pharmacist down the street. And the seniors don’t have much incentive.”
Of course, coupons wouldn’t be so attractive if the co-pays that insurers set weren’t so high. Merritt acknowledges this but said coupons are an inefficient way to make prescription medications more affordable for the people who need help the most.
“These coupons target only those who already have drug benefits. They don’t help the uninsured,” he said, since they cover only a small portion of the drug’s total cost. “[Right now], these are available to Bill Gates as well as to someone who makes $25,000 a year.”
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/drug-coupons/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=24522&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in collaboration with
Dr. Ilse Levin specializes in internal medicine, but you could say she really focuses on incarceration medicine. Levin works at a community health center in southeast Washington, D.C., that pays a lot of attention to treating a population that is often left out of health care: newly released prisoners.

“I have patients who’ve been locked up for 40 years,” Levin says. “They have no idea how to get refills, how to go to a pharmacy. Often, they don’t know how to take their own medications, especially things like insulin.”
When prisoners get out, they often don’t have a job and, therefore, don’t have health insurance. That could be changing soon, though.
The eligibility requirements for Medicaid are expanding in 2014 as a part of the health overhaul law. Right now, Medicaid in most states is mainly targeted toward children, families and the disabled. After the Medicaid expansion goes into effect, even single, adults who don’t have children will be eligible.
Some states and the District have gotten a head start and rolled out the Medicaid expansion early. That means Levin can get reimbursed for the care she provides to patients like Keith Snowden, a D.C. resident who got out of prison last year.
Snowden had been dealing with out-of-control hypertension for years, even before he went to prison in 2009 for selling stolen cars and counterfeit IDs. At his first post-prison visit to Levin’s clinic, his blood pressure was off the charts ? 227 over 153.
“The hospital was right next door. They wouldn’t let me walk next door,” Snowden recalls. “I had to have the ambulance come pick me up. It was that bad.”
Snowden says he had been taking blood pressure medication for years to no effect. Levin conducted a barrage of tests and eventually discovered the culprit: a tumor weighing on his adrenal gland. Snowden had it surgically removed recently; now his blood pressure is back on the charts.
“It took the free doctor for me to go and figure out my problem,” Snowden says. “I really owe my life to her for being so diligent and trying to figure this out.”
Calling Levin a “free doctor” isn’t entirely accurate. Her clinic is run by the charitable non-profit . Doctors and other caregivers there treat patients regardless of their ability to pay, but the kind of life-saving care Levin provided to Snowden costs money.
Levin says it’s much easier to provide appropriate care now that D.C. has moved forward with the health law’s Medicaid expansion, allowing her patients to get health insurance.
“Now, everyone gets Medicaid,” she says. “And suddenly I can get them their medications, I can get them to see a specialist, I can get the studies done. And it is amazing. It’s completely changed my practice.”
Not everyone getting out of prison will be eligible for Medicaid, however. The governors of at least half a dozen states in the Medicaid expansion because it’s too expensive.
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/medicaid-dc-clinic-care-ex-prisoners/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=23479&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>KHN has assembled this resource to show in detail how these positions are taking shape.

Photo by Alex Wong/Getty Images
On Massachusetts Health Reforms, Romney:
- Was a key player in the effort to reform Massachusetts’ health care system. Before his election as governor, he campaigned on a that included the following elements: charging co-pays to higher-income Medicaid recipients to expand coverage, requiring employers of more than to offer insurance or pay a penalty, extending favored prescription pricing in the state’s drug plan for elderly and disabled residents and negotiating an increase in federal funding for Medicaid. In 2005, he proposed , which helped frame the negotiation for health care reforms that ultimately became state law.
- After his term as governor ended, he cited the 2006 state health reform law as a point of , but has since himself from it because it is often considered a for the federal Affordable Care Act, an assertion he rejects. The includes the creation of an online insurance exchange known as the , as well as fines against businesses with more than 10 employees that don’t offer health insurance plans and a mandate that all individuals not covered by public health insurance purchase health insurance.
“If somebody could afford insurance, they should either buy the insurance or pay their own way. … We said: If you can afford insurance, then either have the insurance or get a health savings account. Pay your own way, but no more free ride. That was what the mandate did.” – Romney, GOP candidate debate, Jan. 30, 2008
- Defends Massachusetts’ individual mandate because it was a — not a matter imposed by the federal government.Ìý
“Mr. President, if, in fact, you did look at what we did in Massachusetts, why didn’t you give me a call and ask what worked and what didn’t? … I would have told you, Mr. President, that what you’re doing will not work. It’s a huge power grab by the federal government. It’s going to be massively expensive, raising taxes, cutting Medicare.” – Romney, GOP candidate debate, June 13, 2011
- Advanced a managed care plan for seniors who are eligible for both Medicare and Medicaid.
- Was silent on a 2005 proposal to extend health care benefits provided by the state government to same-sex couples.
- Proposed tort reform in 2006 that would reduce legal fees and make a hard cap of $500,000 on non-economic damages. Lt. Gov. Kerry Healey led this effort.Ìý
“I like what I proposed in Massachusetts when I was governor. And even though the final bill and its implementation aren’t exactly the way I wanted, the plan is a good model. Today, almost every Massachusetts citizen who had been uninsured now has private, free-market coverage, and we didn’t have to raise taxes or borrow money to make it happen. We may find even better ideas in other states. But let’s make certain that conservative principles are front and center. A big-government takeover of health care is the next thing liberals are going to try, and it’s the last thing America needs” – Romney, CPAC Convention, Feb. 27, 2009.
On Medicare & Aging, Romney:
- Favors Medicare reforms that would give future beneficiaries a and allow them to choose between private and traditional plans.
- Maintains that seniors already enrolled in Medicare, or those nearing retirement, would not be affected by his plan, which also would retain a fee-for-service option.
“I wouldn’t repeal it. I’d reform Medicare and reform Medicaid and reform Social Security to get them on a sustainable basis, not for current retirees, but for those in their 20s and 30s and early 50s” – Romney, Tampa Tea Party Debate, Sept. 12, 2011.
- All plans would have to offer coverage at least comparable to what Medicare provides today, though premiums for “traditional” coverage would rise if private companies can provide the same services for less. Critics say that capping the government’s contribution would likely mean that beneficiaries’ costs would increase.
- the December 2011 Medicare proposal by , D-Ore.
- Prior to the Ryan-Wyden plan, supported the Medicare overhaul included in the that was approved by the GOP-controlled House of Representatives.
- the notion that wealthier seniors should pay more toward their health coverage and lower income seniors should receive a higher subsidy.
- Wants to publish a yearly federal balance sheet to help people understand the impact of entitlement spending on the budget and economy.
On The Health Care Marketplace, Romney:
- Wants to strengthen high-deductible health savings accounts by allowing consumers to use them to pay insurance premiums.
- Supports caps on non-economic damage awards in and funds for states to develop other ways to deal with the liability issue, such as health care courts.
- Urges restricting federal regulation of health care insurance, although he supports limited rules to bar insurers from denying coverage to those with when they have had coverage for a specified period of time.
- “co-insurance” plans, in which consumers pay a fixed percentage of the cost of their care.
- Says insurers should be allowed to sell their products across .
- EndorsesÌýending “” and has suggested allowing tax deductions for people who obtain health insurance on their own; also favors allowing individuals and small businesses to join together to buy insurance.
- issue “Consumer Reports”-type ratings of insurance plans.
“The reason health care is so expensive … is not just because of insurance, it’s because of the cost of providing care. And one reason for that is the person who receives care in America generally doesn’t care how much it costs, because once they’ve paid their deductible, it’s free. And the provider, the more they do, the more they get paid … And so what we have to do is make sure that individuals have a concern and care about how much something costs. And for that to happen [we need] health savings accounts. Give people a stake in what the cost of insurance is going to be, what the cost of it is going to be. Co-insurance, where people pay a share of the bill, that makes a difference.” – Romney, Tampa Tea Party Debate, Sept. 12, 2011.
On Health Reform Philosophy, Romney:
- he would allow states to opt out of the federal health law and encourage Congress to repeal it.
- that “each state should be able to fashion their own program for the specific needs of their distinct citizens,” and that states are the “laboratories of democracy.”
- Maintains that “” such as increased competition, provider performance ratings, cost comparisons for procedures, co-insurance and lowering the number of uninsured will improve the health care delivery system.
- Endorses efforts to find an to the fee-for-service payment model.
“I want people to be able to own their own insurance, if they wish to. And to buy it for themselves and perhaps keep it the rest of their lives and to choose among different policies offered from companies across the nation,” he said. “That means the insurance company will have an incentive to keep you healthy. It also means, if you don’t like what they do, you can fire them.” — Nashua, New Hampshire, Jan. 9, 2012
On Medicaid, Romney:
- Opposes the health law’s expansion of Medicaid coverage to as many as 17 million people.
- Supports to allow states to use capped federal contributions to run the program with more flexibility.
- Would and requirements on private insurance and Medicaid coverage.
- Favors reducing the amount of money the federal government spends on Medicaid.
“My view is get the federal government out of Medicaid, get it out of health care. Return it to the states.” – Romney, South Carolina GOP Primary Debate, Jan. 20, 2012.
On Abortion/Contraception Issues, Romney:
- on a promise to not change existing abortion laws, neither making them stricter, nor more lenient. In 2005, he a bill expanding access to contraceptives on these grounds.
- Maintains that Roe v. Wade should be overturned by the Supreme Court so that the abortion issue can be decided by states, but also says that until that happens, Roe v. Wade should be considered the .
- Wants to implement awareness programs in schools.
- against the 2010 health law’s requirement for employers’ health plans to cover contraception without a copayment.
- Opposes for Planned Parenthood.
Romney’s Reaction To Supreme Court Health Law Decision:
- In a after the court’s decision was announced he said that “Obamacare was bad law yesterday, it’s bad law today.”
- Agreed, during , with the Supreme Court that the individual mandate is a tax.
Deep Reads:
:Ìý The Answer Is Unleashing Markets, Not Government
Our divide is fundamental: Republicans believe health care can be best guided by consumers, physicians and markets; Democrats believe government would do better. Some Democrats would have government buy health care for us; set the rates for doctors, hospitals and medicines; and decide what medical treatment we would be entitled to receive for each illness. If you liked the HMOs of the ’80s, you’d love government-run health care…But government can’t match consumers and markets when it comes to lowering cost, improving quality and boosting productivity…The right answer for health care is to apply more market force, not less (Mitt Romney, 05/01/09).
A Sampling Of KHN Video Clips
- Kaiser Health News: Romney Outlines Plans To Replace Obamacare (6/13/12)
- Kaiser Health News: After Winning Nomination, Romney Promises To Rollback Obamacare On Day One (5/30/12)
- Kaiser Health News: Romney Slams Obamacare On Primary Victory Night (4/25/12)
- Kaiser Health News: Romney Calls Health Law ‘Fourth Entitlement’ (1/17/12)
- Kaiser Health News: Romney Quizzed On Contraception During Debate (1/9/12)
:Ìý Preston’s Blueprint
Long before Mitt Romney unveiled his ambitious plan to provide health insurance to everyone in Massachusetts, he hired Ron Preston — “the best health and human services secretary in the nation,” as the governor once called him – to work on a plan to do in the Commonwealth what no other state has been able to do. Romney took the wraps off his vision in November 2004, and Preston, apparently no longer the best health and human services secretary in the nation, was nudged out by the next May.Ìý Preston and a tight group from inside and outside the administration spent six months answering Romney’s basic question: Could it be done? Their answer: Yes, Massachusetts could insure all its residents. But how the Preston working group planned to do it differed, in critical aspects, from what Romney eventually proposed (Bailey, 1/11/06).Ìý
: ‘Romneycare’ Facts And Falsehoods
As the 2012 presidential campaign gets under way in just a few months (believe it or not), we expect to see an increasing number of attacks on so-called “RomneyCare.” So as part primer and part preemptive fact-checking, this article is our attempt to set the record straight (Robertson, 5/25/11).Ìý
: Romney And Health Care: In The Thick Of History
The former governor has faced a fusillade from the right for the plan they call RomneyCare. But a look back at the birth of the Massachusetts law shows why he can’t, and won’t, back away. It was an amazing political feat, and no one’s role was bigger than his (Mooney, 5/30/11).
: ‘RomneyCare’ – A Revolution That Basically Worked
The former governor’s health plan is a policy piñata among his rivals. But a detailed Globe review finds the overhaul has achieved its main goals without devastating state finances. The remaining worry is future costs (Mooney, 6/26/11).Ìý
: Ted Kennedy Helped Shape Mitt Romney’s Career, And Still Haunts It
When Gov. Mitt Romney signed legislation in April 2006 requiring most Massachusetts residents to have health coverage, Sen. Edward M. Kennedy stood by his side, beaming like a proud father. They were onstage at historic Faneuil Hall in Boston, a setting that had a special resonance for the two (Stolberg, 3/24/12).Ìý
: Pride In RomneyCare Shows In Official Portrait
In 2008, for Romney’s official portrait, he had been clear about the image he wanted to convey for posterity. He would be sitting on his desk in front of an American flag, next to symbols of two things he held dear. The first was a photo of his wife, the center of his personal universe. The second was the Massachusetts health care law, represented by an official-looking document with a caduceus–often used as a symbol of the medical profession–embossed in gold on the cover. Romney was deeply proud of the law and felt strongly that it should figure prominently in the portrait, which would hang alongside others dating back to the Colonial era. He wanted to be remembered for that (Kranish and Helman, p. 261-262, 1/17/12).
Other Assorted Video Clips
- : Chris Wallace Interviews Mitt Romney On Healthcare (3/7/2010)
- : Part 2 Of the Wallace/Romney Interview (3/7/2010)
- : Mitt Romney Discusses State Sovereignty And His Replacement Proposal For Patient Protection and Affordable Care Act At University Of Michigan Cardiovascular Center (5/12/11)
- :Ìý Reaction To The Supreme Court Ruling, Plans For Replacement (6/28/12)
: Romney On The Health Insurance Mandate
In 2006, as Massachusetts’ governor, he talked about the state’s mandate in decidedly non-ideological terms: “We’re going to say, folks, if you can afford health care, then gosh, you’d better go get it; otherwise, you’re just passing on your expenses to someone else. That’s not Republican; that’s not Democratic; that’s not libertarian; that’s just wrong” (Liasson, 5/25/12).
: Jonathan Gruber, Health Care’s Mr. Mandate
After Massachusetts, California came calling. So did Connecticut, Delaware, Kansas, Minnesota, Oregon, Wisconsin and Wyoming. They all wanted Jonathan Gruber, a numbers wizard at M.I.T., to help them figure out how to fix their health care systems, just as he had helped Mitt Romney overhaul health insurance when he was the Massachusetts governor. Then came the call in 2008 from President-elect Obama’s transition team, the one that officially turned this stay-at-home economics professor into Mr. Mandate (Rampell, 3/28/12).
: Romney’s Health Care Plan May Be More Revolutionary Than Obama’s
As he pushes to “repeal and replace” President Obama’s healthcare law, former Massachusetts Gov. Mitt Romney has turned to proposals that could alter the way hundreds of millions of Americans get their medical insurance. In public, Romney has only sketched the outlines of a plan, and aides have declined to answer questions about the details. But his public statements and interviews with advisors make clear that Romney has embraced a strategy that in crucial ways is more revolutionary — and potentially more disruptive — than the law Obama signed two years ago (Levey, 4/23/12).Ìý
: Mitt Romney’s Plan May Undercut Mass. Law
A proposal by Mitt Romney to curtail Medicaid spending would dramatically undercut the way the Massachusetts health care overhaul law has achieved near universal coverage. Although the specifics of Romney’s plan are not public, his overall intent – to rein in how much Medicaid money Washington sends to the states – would probably cripple the Massachusetts health care law, which was made possible by an expansion of Medicaid funding. If Romney succeeds, the result could have an ironic twist: the governor who ushered in the country’s first universal health plan would, as president, put in place policies that could undermine one of his signature achievements (Jan, 5/4/12).
This <a target="_blank" href="/news/romney-republican-candidate-on-health-care/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=22597&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]> | Postpartum Depression (Sec. 2952) Urges the National Institute of Mental Health to conduct a multi-year study into the causes and effects of postpartum depression. It authorized $3 million in 2010 and such sums as necessary in 2011 and 2012 to provide services to women at risk of postpartum depression. |
 | Abstinence Education (Sec. 2954) Reauthorizes funding through 2014 for states to provide abstinence-only sex education programs that teach students abstinence is “the only certain way to avoid out-of-wedlock pregnancy, sexually transmitted diseases, and other associated health problems.” Federal funding for these programs expired in 2003. |
 | Power-Driven Wheelchairs (Sec. 3136) Revises Medicare payment levels for power-driven wheelchairs and makes it so that only “complex” and “rehabilitative” wheelchairs can be purchased; all others must be rented. |
 | Oral Health Care (Sec. 4102) Instructs the Centers for Disease Control and Prevention to embark on a five-year national public education campaign to promote oral health care measures such as “community water fluoridation and dental sealants.” |
 | Privacy Breaks for Nursing Mothers (Sec. 4207) Requires employers with 50 or more employees to provide a private location at their worksites where nursing mothers “can express breast milk.” Employers must also provide employees with “a reasonable break time” to do this, though employers are not required to pay their employees during these nursing breaks. |
 | Transparency on Drug Samples (Sec. 6004) Requires pharmaceutical manufacturers that provide doctors or hospitals with samples of their drugs to submit to the Department of Health and Human Services the names and addresses of the providers that requested the samples, as well as the amount of drugs they received. |
 | Face-to-Face Encounters (Sec. 6407) Changes eligibility for home health services and durable medical equipment, requiring Medicare beneficiaries to have a “face-to-face” encounter with their physician or a similarly qualified individual within six months of when the health professional writes the order for such services or equipment. |
 | Diabetes & Death Certificates (Sec. 10407) Directs the CDC and the HHS Secretary to encourage states to adopt new standards for issuing death certificates that include information about whether the deceased had diabetes. |
 | Breast Cancer Awareness (Sec. 10413) Instructs the CDC to conduct an education campaign to raise young women’s awareness regarding “the occurrence of breast cancer and the general and specific risk factors in women who may be at high risk for breast cancer based on familial, racial, ethnic, and cultural backgrounds such as Ashkenazi Jewish populations.” |
 | Assisted Suicide (Sec. 1553) Forbids the federal government or anyone receiving federal health funds from discriminating against any health care entity that won’t provide an “item or service furnished for the purpose of causing … the death of any individual, such as by assisted suicide, euthanasia, or mercy killing.” |
This <a target="_blank" href="/news/10-little-known-health-law-provisions/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=22420&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>The , a global payment model put in place by Blue Cross Blue Shield of Massachusetts in 2009, has both curbed costs and improved the quality of care, according to a published today in the journal Health Affairs.
Global payments, a lump sum toÌýcover all the care of a defined group of patients, are viewed by many experts as a cost-effective alternative to the traditional fee-for-service system.
Massachusetts enacted sweeping state health reforms in 2006 considered by many to be a prototype of the 2010 federal health law, and it with equally dramatic measures to rein in health care spending. The AQC is very similar to the Affordable Care Act’s Pioneer Accountable Care Organization contracts – a part of the Medicare shared-savings program.
InÌýthe state version, 11 health care provider groups were given a fixed budget to care for patients covered by BCBSMA insurance. If the providers stayed under budget, they wereÌýgiven bonuses. If they went over, they had to eat those costs.
After studying data from Blue Cross Blue Shield’s claims and comparing them to claims from doctors not participating in the AQC, the researchers found that – during the second year – providers participating in the global payment system spent an average of 3.3 percent less than the other groups. Those providers who came from traditional fee-for-service contract models achieved the greatest savings – as much as 9.9 percent in year two.
The study also found the participating provider groups achieved quality improvements in chronic care management, pediatric care and adult preventive care,ÌýÌýespecially in year two.
“If these results and improvements continue, the health care system can be put on a sustainable path,” said , the senior author of the study, which was paid for by the .
Chernew noted thatÌýthe findings about the quality of care in the AQC may not be conclusive because “quality measurement is an evolving field.”
For example, he said, one of the main ways providers within the AQC cut costs was by reducing the amount of imaging they did. Chernew said he “can’t say precisely” whether this means they were reducing wasteful imaging or whether they cut back on imaging procedures that could have improved care.
But, he said, the study provides at least some hope that it is possible to rein in the rapidly metastasizing costs of health care without providing a substandard product to patients.
“One way or another, we’re going to have to control spending,” Chernew said. “We as a country simply can’t move forward with the budget trajectory that we’re on. … How will providers respond? Can providers survive in a world where [health care spending] rises more slowly? Our study is optimistic.”
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/study-mass-global-payment-approach-lowers-costs-improves-care/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=3576&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>the matter with kids today? According to the U.S. Department of Agriculture, they’re more expensive.

The USDA released Thursday on how much it costs to raise a child. The grand total for a child born in 2011 is $234,900 — $295, 560 if inflation is factored in — for all child-related expenses, from birth to age 17. That’s a 3.5 percent increase over last year.
The USDA has been keeping track of this since 1960. In that time, how parents have spent their money has changed. One of the two main drivers of the increase is health care costs, which include health insurance premiums not paid by an employer as well as doctors’ visits and prescription drugs not covered by insurance. In 1960 health care costs represented 4 percent of all child-rearing expenses. This year, it represents 8 percent.
However, that’s nothing compared with the exploding cost of education and child care. Spending in that category has gone from 2 percent of child-rearing costs in 1960 to 18 percent now. (On the plus side, the cost of feeding a child has gone down significantly.)
The USDA report also found a disparity in child health care expenses between single-parent families and two-parent families. It estimates that single-parent families with a pre-tax income of $59,410 will spend almost 10 percent less on health care for their children than their two-parent counterparts. On the other hand, it estimates single-parent families who earn more than this amount will spend almost 9 percent more than married parents.
This <a target="_blank" href="/news/costs-of-raising-children-grows-and-health-care-is-a-big-reason/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=3315&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
The good news is that the number of cancer survivors in the U.S. is expected to increase by about 30 percent during the next decade to nearly 18 million, according to a report published this morning by the American Cancer Society and the National Cancer Institute.
The bad news, however, is that people who have survived bouts with cancer in their teens and 20s are much more likely to experience chronic, long-term health problems — even decades after they go into remission. That’s according to .
“Cancer survivors will continue to need some degree of medical surveillance or services they wouldn’t need if they hadn’t been diagnosed with cancer,” said , the researcher who authored the American Cancer Society study. “The growing size of this population will present a challenge to the health care system.”
The CDC researchers found that adults who were diagnosed with cancer in adolescence or young adulthood are twice as likely to be disabled, have chronic conditions, be diagnosed with asthma, and have poor mental and physical health. They’re also more likely to be smokers, to be obese, have high blood pressure, and to forgo health care because of cost, according to the study.
“Health care providers need to be screening these people,” said , the lead author of the CDC study.Ìý“They’re definitely more at risk than the general population for many things.”
Of course, lifelong surveillance of a growing number of cancer survivors could place another burden on an already overburdened health care system — especially on primary care providers, who are responsible for treating patients after they finish receiving care from cancer specialists.
Paul Ginsburg, president of the Washington-based , says these increases in health care costs are an unavoidable consequence of improvements in survival and longevity that have been made for a variety of diseases — cancer being just oneÌýof them.
“People live longer and then other diseases happen to them,” he said. “It’s one of those things where you actually have some cost reductions in the short term from the progress that you make as the treatment becomes more effective, but sometimes it leads to higher spending down the road.”
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/number-of-cancer-survivors-growing-but-so-are-their-health-problems/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=3306&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>
The issue of how to ensure that psychotherapy notes remain private, even from other doctors, was one that troubled many at the second annual in Washington last week.
“Psychotherapists are often the canaries in the coal mine” when it comes to health privacy, said James Pyles, an attorney who specializes in health law at the firm .
Here’s what many say is the problem: If a mental health specialist types up his or her notes from a therapy session and puts them into a patient’s electronic medical record, that file can be shared with any doctor the patient sees within their health system. And, because of a loophole in the , or HIPAA, there’s nothing a patient can do to stop this from happening.
Many mental health professionals, who consider their patients’ privacy and confidentiality to be sacrosanct, find this appalling. But often times, the decision of how they file their patients’ records is not up to them.
Abby Greene is a counselor at a methadone clinic in Long Island, N.Y. Her clinic, which is affiliated with a large psychiartric hospital and health system,Ìýrecently switched over to electronic medical records and now requires all of its clinicians to enter the notes they take during patient sessions into a computer. Greene said she’s thinking about leaving her job because the ethical dilemmas she’s facing are becoming too much to bear.
She said her notes contain details about criminal activities her patients have engaged in. “When I type information into the file and hit send, I don’t feel good,” Greene said. “I feel like this could harm someone.”
A real-life example of Greene’s fears was offered by an attorney named Julie. After being denied treatment for stomach pains by a new doctor, Julie, who spoke at the summit but withheld her last name, discovered that the doctor had full access to her psychotherapist’s notes. The notes contained detailed information about her regimen of psychiatric medications, her diagnosis of bipolar disorder and the sexual abuse she suffered as a child.
expressly prohibits mental health professionals from sharing their psychotherapy notes with anyone if they don’t have their patients’ authorization. However, this only applies if the notes are kept in a separate computer file that isn’t commingled with the patients’ electronic medical record. If they’re not, these detailed narratives are treated just like blood pressure readings or cholesterol levels.
According to Jim Finley at the , behavioral health practitioners have been slow to adopt electronic health records because, unlike with doctors, the federal government didn’t provide them with incentives to adopt. But, in an email, he said his association believes “a substantial number [ofÌýpractitioners] already currently use electronic records and many more are in the process of converting.”
Finley also writes that most of the members of his association are in small private practices, “but practices are consolidating around the country and we expect more of our members to become affiliated with larger integrated models in the future.”
Some health care practices, especially large, organized ones, integrate the medical files for all of their patients into one electronic record. They say this allows their doctors to provide higher-quality, coordinated care.
But , the vice provost for health affairs at the University of Texas at Austin School of Law, says there’s another reason behind the push for IT integration.
“All of this information exists to allow someone to get paid,” he said. “We collect the information we need in order to get paid.”
Â鶹ŮÓÅ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓÅ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/secrets-and-electronic-health-records-a-privacy-concern/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓÅ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=3270&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>