This story was produced in partnership with the╠²
St. Louis —╠²New business opportunities to serve the poor, elderly and sick in an expanding number of states, as well as new ventures outside its core business, drove Centene Corp. last year to record financial heights.
The Clayton, Mo.-based manager of health care for the uninsured and downtrodden broadened its operations last year in Texas, Mississippi, Louisiana and Florida and began serving Medicaid beneficiaries in California, Kansas and New Hampshire.
Centene’s Medicaid Business
- Jury Is Still Out On Medicaid Managed Care
- Medicaid Contractor Centene Was Top Financial Performer In St. Louis
Centene took steps to further diversify by buying a specialty pharmacy company, participating in new health insurance marketplaces, and providing medical care in prisons.
The company also waded into long-term care in the burgeoning “in-home health” services market for the chronically ill and even purchased a stake in a Spanish health management group.
In 2013, Centene was the local publicly held company with the best fiscal performance due to its size, return on shareholder equity, revenue growth and profit growth, a Post-Dispatch analysis concluded.
Centene soared through 2013 by reporting $10.5 billion in revenue, a 37 percent increase over the previous year. Its profits totaled $161.2 million, compared to $1.9 million in 2012 when it reported a large loss related to its discontinued Kentucky business.
Company executives say they are likely to approach $15 billion in revenue in 2014.
“We believe we’re a St. Louis success story,” said Bill Scheffel, Centene’s chief financial officer. “Managed care is a growth industry. … Medicaid is our sweet spot.
“Our compounded growth rate (of revenue) for the last three years is 40 percent,” he said. “We don’t see in the near term any slowdown in growth opportunities.”
Centene employs 9,500 people nationwide, including about 2,000 in the St. Louis area. Its headquarters in downtown Clayton has an on-site medical clinic for workers and a cafe that offers discounts on healthy foods.
The Medicaid contractor’s strong suit is claims processing and its ability to use computer modeling systems to predict with accuracy its members’ health costs.
Still, some patient advocates worry that, to reap greater profits, Centene may clamp down on the quality of care received by its members.
Centene executives say they are committed to improving the health of Medicaid populations.
“We provide quality health care, we save the states money, and we give (the states) budget predictability,” Scheffel said.
Medicaid Expertise
Centene traces its roots to a Medicaid managed care business it started in Wisconsin in 1984.
Since going public in 2001, it has grown into a Fortune 500 powerhouse (ranked 303 last year) that manages state and federal health programs for an “at risk” membership of 2.7 million uninsured and underinsured people in 20 states including Missouri.
“Overall, Centene is one of the most effective players in what is a rapidly growing part of managed care: private providers’ solutions to state health care challenges,” said Tom Carroll, an analyst for St. Louis-based Stifel Nicolaus & Co. Inc. He has given Centene stock a “hold” rating.
Medicaid spending, he added, is one of the largest budget items and challenges for any state.
Centene has “done a very good job of growing the company over the past decade by expanding not only into new states but more recently into new populations within those states,” Carroll said.
Traditionally, Medicaid and CHIP, the Children’s Health Insurance Program, assisted single mothers and children. More recently, Centene has worked with states to broaden the focus to include older, sicker and chronically ill patients on Medicaid.
For example, Centene won a large portion of Florida’s revised Medicaid program, which now includes the aged, blind and disabled. It also provides long-term care in the Sunshine State.
Its new contracts in Michigan, Ohio and South Carolina include health coverage for “dual eligibles” ŌĆö low-income seniors and people with disabilities who are enrolled in both Medicaid and Medicare.
Centene’s contracts in states such as Illinois have expanded to include care coordination, optometry, behavioral health and pharmacy benefit management services.
Beginning in 2013, Centurion ŌĆö Centene’s joint venture subsidiary with MHM Services Inc. ŌĆö has won contracts to provide mental health and preventive health services to 41,000 inmates in prisons in Massachusetts, Tennessee and Minnesota. These new efforts give Centene experience in operating point-of-care clinics.
Centene has Medicaid contracts in 14 states including Louisiana, Texas and Missouri.
“Centene’s contract pipeline through 2014-15 remains robust,” Sarah James, an analyst at Wedbush Securities in Los Angeles, wrote in a recent report.
Wedbush has given Centene stock an “outperform” rating, based on its view that it will benefit significantly from Medicaid expansion.
Three of the states where Centene serves Medicaid populations ŌĆö California, Massachusetts and Washington ŌĆö are expanding their programs. As more states decide to expand their programs, Centene is expected to benefit from enrollment increases.
Centene has captured 14.6 percent of the managed care market for at-risk residents in Missouri, where the Legislature has refused to expand the Medicaid program. Centene’s subsidiary, Home State Health Plan, provides health services in 54 Missouri counties to 59,200 uninsured people.
The two other managed care providers for Missouri Medicaid are Tampa-based WellCare Health Plans Inc. and Healthcare USA, a Coventry unit owned by Aetna Inc.
Wedbush’s James said new business is likely to account for 21 percent of Centene revenue in 2014.
Centene is participating in health insurance exchanges in nine states and plans to expand its offerings in these states in 2015. About 80 percent of its enrollees are low-income residents who are eligible for federal subsidies, but not for Medicaid.
But the company’s expected enrollment of about 70,000 people this year on the health exchanges is expected to have only a minimal impact on its financial performance.
“While enrollment is small in the exchanges, they showed an ability to develop and deploy a new health insurance product ŌĆö targeting folks who don’t qualify for Medicaid but are living close to the edge,” Stifel’s Carroll said.
Some of Centene’s success can be chalked up to vertical integration.
“Centene has been very acquisitive over the years,” Carroll said. “It’s acquired the right tools to effectively serve a Medicaid population.”
For example, Centene’s behavioral health subsidiary, Cenpatico, provides mental health services to 156,000 members in Arizona and also provides services in other states. The Medicaid population has high rates of mental illness.
In 2013, Centene acquired AcariaHealth, an Orlando, Fla.-based specialty pharmacy company.
AcariaHealth is one of the largest distributors of Solvaldi, a new and highly expensive Hepatitis C drug that has spiked medical costs for other Medicaid providers. Centene’s new ownership of AcariaHealth, however, has offset the expense of Solvaldi.
“That’s a great example of how Centene is managing the population well and dealing with a new, high-cost drug,” Carroll said. “It looks brilliant on Centene’s part.”
(St. Louis County-based Express Scripts Holding Co., a pharmacy benefit manager, has reacted to Solvaldi’s high costs by forming a coalition to boycott the drug once a competitor reaches the market.)
In January, Centene acquired a majority stake in U.S. Medical Management, which provides in-home health services to high acuity populations. In April, Centene agreed to purchase a noncontrolling interest in Ribera Salud S.A., a Spanish health management group that is widely regarded for its public-private health care partnership model.
Scheffel said the transaction represents Centene’s “initial foray into the international” sphere in which the company will gain valuable experience.
Keith Williamson, Centene’s general counsel, also attributed Centene’s continued success to a corporate culture that embraces “flexibility, innovation, entrepreneurship and high standards” as well as civic engagement and volunteerism.
Risk Factors
According to the federal Centers for Medicare & Medicaid Services, the total Medicaid and CHIP market was about $408 billion in 2011; the market is estimated to rise to $839 billion by 2022.
Indianapolis-based WellPoint Inc. has the largest number of Medicaid members, followed by Minnesota-based UnitedHealthcare. Centene, which is No. 3, faces stiff competition from Long Beach, Calif.-based Molina Healthcare Inc. and WellCare.
Despite its success, Centene depends heavily on state governments and its ability to retain key contracts for its revenue.
Its managed care subsidiaries in Texas, for instance, represent 37 percent of Centene’s revenue from its continuing operations in 2013. Centene serves one quarter of the Texas market for managed care of at-risk populations. Its members there total about 935,100 people.
As a government contractor and “price taker,” Centene has a high exposure to changes in state budgets and rate setting. The company’s risks also include unexpected changes in medical costs or the utilization of these services.
It can also be dicey entering new states. Centene ran into trouble in Kentucky, where ŌĆö according to Centene executives ŌĆö rates were set based on health data that underestimated true costs.
After negotiations to raise its rates faltered, Centene last year terminated the contract.╠²Litigation between Centene and the Commonwealth of Kentucky continues over whether the company had the right to end the contract a year before it was set to expire.
A loss for Centene could cost the company as much as $46 million, Scheffel said.
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/medicaid-contractor-centene-was-top-financial-performer-in-st-louis/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33804&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with the
WellPoint Inc., the parent of Anthem Blue Cross and Blue Shield in Missouri, took a huge gamble when it dove headfirst into many of the new health insurance marketplaces around the country.
Aetna Inc. hedged its bets by entering a patchwork of federal- and state-run health exchanges, but skipped California and New York, two of the most populous markets.
UnitedHealth Group Inc., the nation’s largest health insurer, decided to participate in only a dozen or fewer exchanges in 2013. Given the current disarray on the federal-operated website, its strategy may prove wise ŌĆö or overly cautious.
In business, it’s usually best to be first to enter and carve out a new market. Occasionally, being first can be a costly, even crippling, mistake. And the health insurance industry, hemmed in by the new health law’s underwriting rules and administrative spending limits, has not faced this level of risk for decades.
It’s far too early to identify which insurers will be winners or losers under the Affordable Care Act. Mired by weeks of computer malfunctions, the slow-motion rollout of healthcare.gov will only prolong the agony of insurance executives who have long grown accustomed to carefully controlled risk.
The latest wrinkle: President Barack Obama’s move on Thursday to rescind the cancellations of millions of policies that don’t conform with the new law.
It’s becoming clear now that it may take some time, perhaps until at least 2015, for key aspects of the Affordable Care Act to start working, including the new health insurance marketplaces, say health insurance brokers and consultants.
Despite the uncertainties, the major insurance companies are publicly taking many of the changes in stride.
The “big five” ŌĆö UnitedHealth, WellPoint, Aetna, Humana and Cigna ŌĆö recently announced strong third quarter results, and analysts are expecting modest gains overall in 2014. In those quarterly reports, the top five posted increased revenue; two ŌĆö Aetna and Cigna ŌĆö reported increased net income.
They’ve wrapped their arms around the idea that Obamacare, for better or worse, is the law of the land.
“The health exchanges are here to stay, and we will be part of them,” Steve Walli, chief executive of a UnitedHealth subsidiary’s operations in Missouri and the River Valley, said in a recent interview. “We certainly plan to participate in many of these exchanges for 2015. … There will be a lot of people insured in the health exchanges who’ve never had insurance before, and we’ll have some attractive options for these people to consider.”
Treading Cautiously
Yet the law may unleash changes that could undermine the top insurers.
A Deloitte consulting study, released in 2012, concluded that the new health law may significantly disrupt the insurance industry.
The law “could increase the market size for individual health insurance by more than five-fold by 2020, raising the number of individual policy holders to approximately 72 million in 2020,” according to the Deloitte study.
That larger individual market could entice banks, smaller insurers and large retailers to enter, Deloitte found. “The door is opened to a full-scale disruption of incumbent group carriers by smaller, more nimble upstarts.”
Wendell Potter, a former insurance executive turned industry watchdog and consumer advocate, also has speculated that the new exchanges may prove to be the undoing of major insurers.
In a Sept. 30 column for the Center for Public Integrity in Washington, Potter predicted the insurance giants will have a hard time competing against smaller players, including nonprofit insurers, in the exchanges. Many consumers, he wrote, will eventually conclude they don’t need a behemoth to serve as a “middleman” to health providers.
Potter, who worked previously as an executive for Cigna and Humana, shocked the industry in 2010 with his tell-all book, “Deadly Spin.” He contends the new law “will signify the beginning of the end of the health insurance industry as we know it.”
An Uncertain Frontier
Insurance companies have vast amounts of public and private data about consumers’ medical claims histories, but cannot predict with certainty whether enough healthy young adults will buy policies to offset older consumers and those with chronic conditions.
Many young adults may choose to absorb the first year’s small penalty ŌĆö $95 or 1 percent of income, whichever is greater ŌĆö rather than pay more than $1,000 a year for a low-cost, catastrophic health plan.
“For these new reforms to work, you need broad participation in the health care system,” said. Robert Zirkelbach, a spokesman for America’s Health Insurance Plans, a Washington-based industry trade group. “If young, healthy people choose to wait and purchase coverage when they need it, that’s going to drive up the cost of coverage for all.”
Vincent Blair, a health insurance broker in Webster Groves, questions how insurers will be able to absorb the cost of caring for the previously uninsured and tough to insure. “I don’t see how it works,” he said.
“Overwhelmingly, the people who are calling me about policies on the exchange are sick,” he said. “These are people on growth hormones at $4,500 a shot or who have rheumatoid arthritis and each shot costs $4,800. … It takes a lot of healthy people to cover these shots. Is there enough underwritten business on the insurers’ books to pay for all that? Will that temper the blow?”
Insurers Push Back
Under the Affordable Care Act, the insurers cannot exclude customers with pre-existing medical conditions, and policies must also include “minimum essential benefits,” including maternity care, mental health care and preventive care such as mammograms and colonoscopies ŌĆö costly benefits that were not previously required.
To stay profitable, insurers have designed products with higher deductibles and higher out-of-pocket limits. With more “skin in the game,” consumers are being nudged toward making health care choices that are cost-efficient.
Insurers such as Anthem have also become aggressive in narrowing their health provider networks to exclude hospitals and physicians who tend to charge higher rates. Winnowing providers can reduce an insurer’s medical costs, but decreases consumer options.
In Missouri, Anthem plans to exclude BJC HealthCare ŌĆö which operates Barnes-Jewish Hospital, St. Louis Children’s Hospital and several other hospitals in the St. Louis area ŌĆö from its network for 2014 individual policyholders. The other insurer on the state exchange, Aetna subsidiary Coventry Health Care Inc., is offering a tiered plan here: Consumers with a broad network including BJC HealthCare pay higher monthly premiums; those with a narrow network without BJC pay lower premiums.
Consumer advocates say that some insurers are taking actions that may harm consumers.
In a Nov. 6 letter, Connecticut Attorney General George Jepson asked the U.S. Department of Health and Human Services to “aggressively scrutinize” what he described as a UnitedHealth subsidiary’s decision to drop a significant number of doctors from its Medicare Advantage plans.
America’s Health Insurance Plans, meanwhile, has supported bipartisan legislation to delay implementation of the health insurance sales tax, which will collect an estimated $8 billion in 2014 and raise the cost of individual premiums. AHIP also has lobbied against federal cuts that could increase costs and reduce benefits of Medicare Advantage plans for seniors.
A Cheery Outlook
During an earnings call last month, top executives from WellPoint seemed buoyant.
“We remain optimistic about the long-term membership growth opportunity through exchanges,” Joe Swedish, WellPoint’s chief executive, told Wall Street analysts, according to a transcript by Thomson Reuters. “That said, it will likely be some time before we can get an accurate picture of what our initial volume on exchanges could be in 2014 and what the resulting risk profile might look like.”
WellPoint plans to spend up to $100 million by the end of the year to market its new policies ŌĆö once the federal government fixes its HealthCare.gov website to make it easier for consumers to sign up.
As their companies continue to thrive, top insurance executives are enjoying generous pay packages.
UnitedHealth CEO Stephen Hemsley, for example, received $13.9 million in 2012, according to the company’s proxy filing with the Securities and Exchange Commission.
Aetna’s chief executive, Mark T. Bertoli, was paid $13.3 million in 2012.
WellPoint’s former CEO Angela Braly received more than $20 million in 2012, the year in which she resigned in August. Swedish became CEO in March, after John Cannon served on an interim basis.
Can the insurers’ heady days last forever? Under the new law, insurers face “medical loss ratio” restrictions on their administrative expenses. They must spend at least 80 percent of premium dollars on medical care ŌĆö or provide a rebate to customers. The rule is 85 percent in large group markets.
As the nation’s largest insurer, Minnesota-based UnitedHealth’s core strength is its high degree of diversification in providing coverage and management services to companies of all size as well as millions of seniors on Medicare Advantage plans, poor people on Medicaid programs and individual policy holders.
But would UnitedHealth and its rivals prefer to operate in an arena that has fewer uncertainties?
“We’re in a highly competitive business. Managing risk is not an easy thing to do,” Walli said. “(But) this company was built on risk. We love to manage risk, and we think we’re pretty good at it.
“Any one of my customers can go somewhere else if I try to charge too much,” he said. “And the Affordable Care Act has produced new forces of competition.”
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/health-insurers-face-uncertainty/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26065&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with the
ST. LOUIS — Some children who visit Grace Hill’s dental chairs at the Murphy-O’Fallon Center in north St. Louis arrive in such terrible condition that all their teeth must be pulled.
For young, unemployed men, an appointment at one of Grace Hill’s four neighborhood health centers may be their first doctor’s visit in several years.
Pregnant women receive medical care at Grace Hill and also learn valuable health lessons in group sessions.
Grace Hill Health Centers Inc., a nonprofit charitable organization that relies heavily on the federal government, provides primary health care for the poor and uninsured in the St. Louis area.
Its spacious, well-appointed health centers ŌĆö each offering a full suite of medical services under one roof ŌĆö not only relieve pressure on area hospital emergency rooms, but also forge stronger community ties, helping to stabilize crime-ridden neighborhoods.
Community health centers such as Grace Hill are a linchpin of President Barack Obama’s administration’s efforts under the Affordable Care Act to eventually contain the nation’s health care costs by providing cost-effective, primary care to the poor.
But key government funding for Grace Hill and other smaller nonprofit community health centers in St. Louis is in jeopardy, while the number of people in need of free and discounted care continues to rise.
“You can’t provide the same amount of care with dollars being pulled out of the system,” said Robert Fruend, executive director of the St. Louis Regional Health Commission. “These places run lean and tight. There’s no fat in these health centers. So when you cut, you cut bone and actual service. … Everything’s on the table in D.C. right now.”
At least 17 percent of Grace Hill’s annual budget of $33 million will evaporate unless the federal government decides to extend its “Gateway to Better Health” program, a demonstration project intended to help uninsured residents transition to an expanded Medicaid program.
If the Gateway program funding is eliminated, Fruend said, uninsured patients “will have to figure out where to get care. … Then, the emergency rooms get more crowded. It starts that vicious cycle all over again that we were able to get away from 10 years ago.”
An additional 33 percent of Grace Hill’s budget is contingent on federal grant programs that also have come under intense scrutiny as part of the nation’s fiscal crisis.
These threatened cuts come as St. Louis ConnectCare, a key provider of specialty medical services to the area’s poor since 1998, is preparing to lay off more than half of its staff.
The Gateway program was designed as a short-term bridge, but with state lawmakers refusing to expand Medicaid, federal health officials are left in a bind.
Why should the average citizen support health care for the poor?
“It’s the right thing to do,” Fruend said. And by providing less expensive primary and preventive care at neighborhood health centers rather than costly emergency care at hospitals, he added, it helps holds down the cost of health insurance for everyone. In serving the uninsured, health systems such as BJC HealthCare and SSM Health Care tend to shift a portion of these higher costs to patients who have private insurance.
Fruend also said that anyone ŌĆö even full-time employees ŌĆö may one day fall into circumstances in which they, too, need subsidized health care. Many people these days are living just one paycheck away from charity.
“Healthier citizens over time cost the health care system less,” said Alan Freeman, chief executive of Grace Hill. “An investment in primary care helps to avoid medical crises down the road.”
A Mission
Grace Hill is the St. Louis area’s largest provider of outpatient services to those on Medicaid and also serves a disproportionate amount of the area’s uninsured and underinsured.
Its neighborhood health centers offer primary care, internal medicine, obstetrics and pediatrics as well as pharmacy and dentistry services, a child development center and access to an adult psychiatric clinic.
Men ages 19-64, especially those with chronic illnesses, would be among the first patient groups at Grace Hill to be affected by substantial funding cuts.
Because these patients often suffer from chronic diseases such as asthma, hypertension and diabetes, they rely on frequent doctor’s visits and low-cost medications.
Grace Hill patients pay a sliding scale fee, starting at $10 per prescription, a $20 co-payment for a doctor’s visit, and a $35 co-pay to see a dentist. Patients also enrolled in the Gateway program pay only $1 to $3 for doctor’s visits and $3 or less for prescriptions. As a result, they have much greater adherence rates for taking their medications and showing up at follow-up appointments.
In addition, Grace Hill provides primary care, prevention and maintenance for nearly 3,000 adults who have a serious mental illness, from bipolar disorder to schizophrenia. These patients live and function in the community with the help of outpatient services, but are often stricken with high anxiety and vulnerable to psychiatric crises including extreme depression and psychosis.
“We have to treat the person as a whole,” said Rajeev John, Grace Hill’s manager of clinical social work. “We also try to preserve their general health.”
These mentally ill patients are often taking two or three potent medications, some with strong side effects. They are often homeless, have short life expectancy and are prone to pneumonia, bronchitis, diabetes and sexually transmitted diseases.
Grace Hill has a partnership with Washington University School of Medicine on adult psychiatric care at the BJC Behavioral Health facility on Olive Street.
If Grace Hill’s federal funding is cut, experts say, more patients are likely to show up at emergency rooms suffering from panic attacks and psychosis. Many psychiatrists are unwilling to see mentally ill patients who are uninsured or on Medicaid.
Dr. David Richards, who practices internal medicine at Grace Hill, says that he often sees signs of poverty in his patients and needs to double up as a psychiatric counselor.
“We see a lot of very sick people here,” he said, adding that patients in general have high rates of obesity and low rates of health literacy. “The overwhelming majority of my patients have next to no teeth. … Some people are not able to afford coats in the winter.”
Grace Hill patients also produce about 800 babies a year, most of which are delivered at Barnes-Jewish Hospital and SSM St. Mary’s Health Center. Grace Hill’s “centering pregnancy” sessions are credited with holding down the number of preterm deliveries and babies with low birth weights.
Some young children who receive care at Grace Hill’s Murphy-O’Fallon Clinic show signs of homelessness.
“They move a lot, following their parents,” said Dr. Amal Antoun, a pediatrician at the center. “If I see a kid for a health issue, and I see that they have another health issue, we handle that immediately, because I know that I may not see them again. That’s my chance.”
Many of these children suffer from asthma, which can be triggered by environmental conditions such as second-hand smoking, soiled carpets and roaches. A rising number of children in grade school are obese and diabetic.
“I did my residency at City Hospital and worked with this population,” Antoun said. “I felt I could do something for these kids, make them feel better. I see them growing and some of them going to college, and that makes my day.”
In north St. Louis, Grace Hill also operates the Water Tower Health Center. Its other facilities include the Soulard-Benton Center and Grace Hill South Center on South Broadway, which has a high Latino population.
According to Grace Hill officials, about 95 five percent of Grace Hill’s patients have income below 100 percent of the federal poverty level, and roughly 60 percent are uninsured. About 36 percent of Grace Hill’s patients are on Medicaid or the Children’s Health Insurance Program (CHIP) for children, and 22 percent are homeless or staying in community shelters.
“The majority of our clinicians see this as a mission, and in some respects a ministry,” said Freeman, Grace Hill’s director. “It’s their way to give back, and I have a great respect for them.”
“We place an emphasis on the team environment,” he said, “so we have a number of advanced nurse practitioners work in collaboration with one or more clinicians on staff.”
Grace Hill has 320 employees, including 17 physicians, 10 nurse practitioners and five psychologists. It also employs eight dentists and four dental hygienists. And it plans to operate a large-scale dental clinic near Lafayette Square in St. Louis in conjunction with A.T. Still University in Kirksville.
Grace Hill also provides optometry services in partnership with the University of Missouri at St. Louis; audiology services through the nonprofit Center for Hearing & Speech; and foot care through for-profit Midwest Podiatry Services.
Obese patients receive one-to-one counseling and referrals to the clinic’s dietitians. Group sessions are also held on smoking cessation and diabetes.
“We’re trying to prevent our patients from hitting bottom and keep them as stable as possible,” said Yvonne Buhlinger, Grace Hill’s vice president of community health services. “This is their primary care home.”
The Most Vulnerable
Grace Hill is one of four “federally qualified health centers,” or FQHCs, in the St. Louis area and one of the largest of 23 of these centers statewide. The others in St. Louis are Betty Jean Kerr People’s Health Centers; Family Care Health Centers; and Myrtle Hilliard Davis Comprehensive Health Centers Inc.
Under the law, these community health centers exist mainly to serve vulnerable populations. They are required to provide care to all patients, regardless of their ability to pay, and must offer a sliding fee scale based on income.
FQHCs, which are found in urban and rural areas, must be run as nonprofit entities and governed by community-based boards in which the majority of directors are consumers or patients.
“We can’t just give someone a prescription and quick instructions,” Buhlinger said. “When you become our patient, you don’t just see the doctor. You’re going to be contacted and followed up on.”
She said that many patients needed education, monitoring and scheduling. In some cases, she added, a home visit may be warranted.
Grace Hill’s neighborhood centers handle a total of nearly 47,000 individual patients (adults and children) a year for primary care at its four comprehensive health centers and BJC Behavioral Health, and about 135,000 total patient encounters.
Freeman said that in the past five years Grace Hill had seen an increase of about 11,000 patients.
Grace Hill is trying to alleviate patients’ barriers to care, arranging transportation for some patients and establishing later clinic hours for working people.
“People have the notion that we’re kind of a mom-and-pop shop. We are a state-of-the-art health care facility,” said Veronica Richardson, Grace Hill’s vice president for quality improvement. “We want to be the health provider of choice.”
She said that Grace Hill’s strength was its “sense of community,” a multi-generational presence in north St. Louis for more than a century.
“Here, you see people who you know who live in the neighborhood,” she said. “Sometimes, you go upstairs (to the clinic’s main floor) and it’s just like old home week.”
But it also can be a tough job, with patients sometimes voicing their frustration and anger over their circumstances to Grace Hill’s staff.
“People who work in a community health center have a calling,” Richardson said. “You do it because you want to take care of those who don’t have a voice and need to be heard.”
But with today’s financial uncertainty and increased competition in the health care marketplace, Grace Hill is beginning to focus on how to make its neighborhood centers even more attractive to patients.
“We’re committed to state-of-the-art services for our patients,” Buhlinger said. “We strive to provide the highest quality of care that is the most accessible.”
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/clinic-funding-in-jeopardy/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26499&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with the
North St. Louis County, Mo. —╠²On a recent weekday afternoon, Christian Hospital ambulances raced to a car fire on Interstate 270, a patient’s cardiac arrest and a man with a knife wound.
Other private ambulances, as well as those operated by the cities of Hazelwood and Florissant, also delivered dozens of patients to the north St. Louis County hospital that day.
“I’ve looked out and seen 10 ambulances at one time, lined up to get in,” said Chris Cebollero, chief of Christian’s emergency medical services.
Rarely in the public eye, Christian Hospital operates the busiest emergency department in the St. Louis area, with more than 110,000 annual visits ŌĆö more than 300 a day on average ŌĆö at the hospital’s main campus and its affiliate, Northwest HealthCare. The Christian emergency department serves more Medicaid and uninsured patients than any other area hospital’s ER, according to the St. Louis Regional Health Commission.
“Christian Hospital is the major safety net provider of care for a vast majority of our region right now,” said Robert Fruend Jr., the commission’s executive director. “They have an incredibly large service area, from Illinois to North County. There aren’t many community health centers or hospitals around Christian right now, and the number of families in poverty in that area has skyrocketed.”
Christian’s ongoing struggle to serve the disadvantaged is not likely to get any easier under the Affordable Care Act. Federal and state reimbursements and “disproportionate share” payments to hospitals that treat a greater percentage of the poor are being reduced. And with Missouri’s reluctance to expand its Medicaid program, federal dollars are expected to get even more scarce.
But the success or failure of health reform will hinge in large part on efforts by overburdened hospitals such as Christian to find the most cost-efficient ways to serve the poor.
Christian’s emergency room is often jammed with dozens of adults and children. Many patients are walk-ins, and hospital officials estimate that as many as 40 percent of patients are using the ER for primary care and urgent care, rather than true emergencies.
“Some people believe our unemployment in North County is double the state rate, and those people come into the ER when they need to be treated,” said Ron McMullen, president of Christian Hospital, which has more than 400 physicians and about 2,100 employees.
He said there are times when the community hospital is overwhelmed by its high volume of patients, but adds, “We try to get people in and out very quickly, and we usually do it pretty well.”
Similar to any other ER, patients are triaged: a patient who suffers a heart attack gets seen quickly; someone with a twisted ankle must wait.
To reduce demand on ER services, Christian has succeeded in hiring a few additional primary care physicians. “If we hadn’t done that, we would have been flooded,” McMullen said.
Christian, one of 13 hospitals in the BJC HealthCare system, logged 112,117 emergency department visits last year ŌĆö almost 14,000 more emergency visits and trauma cases as Barnes-Jewish Hospital. That figure includes Christian’s 28-acre campus on Dunn Road (near the intersection of Interstate 270 and Highway 367) and its 24-hour emergency care facilities at Northwest HealthCare in Florissant.
Christian’s main campus offers a fairly comprehensive range of services, from cancer, stroke and heart care to 14 surgery suites, psychiatry and orthopedics. But, except in emergencies, it no longer delivers babies. DePaul Health Center provides obstetric services in North County.
In addition to its emergency room, Northwest HealthCare has imaging and laboratory services, physical and occupational therapy, and centers for breathing and sleep disorders.
Changing Economy
For more than a century, Christian has served North County’s diverse population of working-class families and the poor. But many of the steady factory jobs that fueled the area’s economy have disappeared since the 1980s, and the recent recession compounded the pain, leaving the hospital in a precarious financial position.
“We’ve seen the financial viability of the hospital diminish,” McMullen said. “What’s put Christian in trouble in recent years is the migration of (paying) patients away from North County, leaving more people with little or no health insurance. … In effect, BJC subsidizes the care at Christian from some of its other hospitals.”
In the past two decades, residents with blue-collar jobs and health insurance coverage moved away from North County, many relocating to St. Charles County. At the same time, residents of the city of St. Louis, many poorer and without health insurance, moved in.
According to a 2011 study sponsored by the St. Louis County Health Department, 26 percent of males in North County have no usual source of medical care ŌĆö a high percentage compared to other study regions.
That demographic shift also left North County’s population hollowed out, with fewer middle-aged wage earners and more senior citizens and children. And with the financial downturn, many area residents lost their jobs and health insurance.
“It is hard to get a physician to take a low-income, uninsured person, period,” Fruend said. “Our community health center networks haven’t yet expanded fully north to meet the changing needs of our population.”
Christian officials said that 50 percent of their patients are on Medicare; 16 percent are on Medicaid; 23 percent are privately insured; and 11 percent are “self-pay” or uninsured. In addition, a substantial portion of patients’ accounts are classified as “bad debt” because they do not pay their bills. In the emergency department, more than half the patients are uninsured or on Medicaid ŌĆö the highest proportion in the St. Louis area except for its two leading children’s hospitals.
The sum of these circumstances has left Christian, which has an average census of about 255 patients, performing the functions of a tax-supported public hospital. Unlike most metropolitan areas, St. Louis no longer has any public hospitals. In 1979, city officials closed Homer G. Phillips Hospital; St. Louis City Hospital closed in 1985, and St. Louis County Hospital closed a year later.
Since 2000, three free-standing hospitals in the greater St. Louis area that served large populations of uninsured patients have closed: Forest Park Hospital, Normandy Community Hospital, and Kenneth Hall Regional Hospital in East St. Louis.
Revenue from the other 12 hospitals in the BJC HealthCare system, including Barnes-Jewish Hospital, subsidize a substantial portion of Christian’s operations, according to Steven Lipstein, president and chief executive of BJC.
“BJC provides the funding to support (Christian’s) operating loss plus any additional cash requirements that the hospital has,” Lipstein said. “Without BJC-like organizations that can pool together revenue and expenses, it would be difficult to sustain important community assets such as Christian Hospital as stand-alone hospitals.”
Last year, Christian had revenue of $275 million and an operating loss of $17 million, according to hospital officials. In the first six months of this year, Christian had revenue of $125 million and an operating loss of $14.6 million. Those figures exclude any investment income or loss.
“Christian Hospital is a very well-run hospital, and it’s been well-capitalized over the years,” Lipstein said. “But over the last decade, the hospital’s unreimbursed care and free care (its charity care and bad debt together) has grown from $15 million in 2002 to about $32 million in 2012.”
It’s a Catch-22. Any failure by health providers to serve the poor, including preventive care and professional attention to ongoing illness, results in a sicker population with more chronic conditions and higher treatment needs ŌĆö and ultimately, greater health care costs for institutions and taxpayers to absorb.
In the last decade, BJC HealthCare has poured $173 million of investments into Christian. Since 2002, those funds have gone toward such projects as rebuilding the hospital’s kitchen, renovating patient floors, buying new medical equipment, and building Northwest Healthcare on the site of the former Christian Hospital Northwest. About 30 percent of Northwest Healthcare’s emergency patients are children.
“BJC’s game plan is to continue to use all available sources of revenue to help us sustain our mission at Christian Hospital,” Lipstein said, “and to continue to advocate that everyone who lives in America should have health insurance.”
Quality Of Care
Christian Hospital is a spacious, well-appointed hospital with a large intensive care unit, a diabetes center, a psychiatric ward, a surgery center that performs about 6,000 surgeries a year and a cancer resource center geared toward patients recently diagnosed with the disease ŌĆö and their families.
It draws favorable reviews from its patients, 62 percent of whom told independent surveyors they would “definitely recommend the hospital,” according to the Hospital Compare website sponsored by the federal Centers for Medicare & Medicaid Services.
Christian’s readmissions and death rates for heart attack, heart failure and pneumonia as well as serious complications are within the national average, the website says, and its rate of central line-associated bloodstream infections is “better than the U.S. national benchmark.” Christian’s deaths among patients with serious treatable complications after surgery and also its rate of serious bedsores per patient are worse than the U.S. average.
“Christian is one of the most efficient operations in all of BJC Healthcare,” BJC’s Lipstein said. “When it comes to clinical staffing, Christian meets all the community standards for outstanding medical care.”
But like other hospitals in the St. Louis area, many patients at Christian Hospital’s emergency room wait for long periods of time.
According to Hospital Compare, Christian’s patients spend 6 hours, 6 minutes on average in the emergency room before being admitted as an inpatient; 2 hours, 9 minutes on average after a doctor decides to admit them as an inpatient; 42 minutes on average before being seen by a doctor or nurse; and 1 hour, 6 minutes on average to receive pain medication after arriving in the ER with broken bones. These times exceed the Missouri average and the national average.
McMullen said that Christian’s quality of care is in the top 25 percent of hospitals nationally among community hospitals. He said that Christian’s main campus is well within the national average of those patients who leave the ER before being seen by a health care professional, and within the top 10 percent nationally at Northwest Healthcare.
But to ease congestion, Christian is undergoing a $17.3 million expansion of its main emergency department.
Christian’s charges are higher than its nearby competitors, to compensate for its high cost of charity care and bad debt. For example, Christian’s average charges for cardiovascular surgery are $94,202, compared to $78,100 at St. Mary’s Health Center in Richmond Heights, according to the American Hospital Directory.
“We want to do what’s necessary to keep the northeast campus of Christian Hospital physically viable until about 2040,” McMullen said. “At some point, the public sector is going to have to step up to the plate to make sure the financial viability and physical viability of the hospital is there. ŌĆ” We’re going to need to have a public or political discussion about the future of and availability of hospital care in North County.”
Ideally, McMullen said, patients would rely more on primary care physicians, and public health care dollars would follow an uninsured person to any hospital the patient visits.
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/struggles-of-christian-hospital/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=27003&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from our partner the
When the new health exchange opens for business in Missouri on Oct. 1, at least three major health insurers will not be participating.
UnitedHealthcare, the nation’s largest insurer, said Monday that it won’t offer insurance policies this fall in the federally run health exchange in Missouri, but may enter the exchange later. The Minneapolis-based insurer also plans for the time being to stay out of Illinois’ health exchange.
Cigna, another leading insurer, intends to participate in only five of the 10 states in which it currently writes individual health policies. Cigna, based in Bloomfield, Conn., does not write individual policies in Missouri. Assurant Health, based in New York City, also won’t participate next year.
Health exchanges are designed to give consumers the opportunity to “comparison shop” for health insurance plans, and some insurers have complained there are still too many uncertainties to make sound business decisions.
But the Blue Cross and Blue Shield Association, which represents state-based Blue Cross plans nationwide, appears to be getting set to make a big splash in many of the new exchanges. The association has partnered with the nation’s largest drugstore chain, Walgreen Co., based in Deerfield, Ill., to launch a national educational campaign to better acquaint consumers with their health coverage options.
The decisions by some insurance industry giants to withhold their participation in certain state and federal health exchanges may be interpreted as another setback for the roll-out by the administration of President Barack Obama of a key component of the Affordable Care Act.
Insurers that already have a big foothold in the individual market and want to protect and perhaps expand their market share are jumping in, while others whose mainstay is writing policies for employees of larger companies are counting to three before they take the plunge.
Leading health policy experts say they are not alarmed.
“Everyone expects this will take some time to ramp up and that enrollment may not peak until year two or three,” said Larry Levitt, a senior vice president at the Henry J. Kaiser Family Foundation, a nonprofit, nonpartisan health policy research group. (KHN is an editorially independent program of the foundation)╠²“So it’s a business strategy decision of whether to jump into the market from day one and capture market share, or wait a year or two until things shake out.” He said that insurers were “making very individualized decisions about whether they participate and where they don’t.”
Such decisions, Levitt said, depend on an insurer’s brand-name recognition in a state and its contracts with doctors and hospitals. He also said that, because such companies will need to invest heavily in the direct marketing of exchange-related policies, they must expect enough of a market share to justify the investment.
What matters, he said, is that consumers have enough choice of individual health policies and there is enough competition among insurers to help drive premiums down.
“As long as you’ve got at least three (insurance) plans in an area, you’re doing fine,” he said.
John Holahan, a fellow at the Urban Institute in Washington, said he anticipated that “there will be vibrant competition, except in the states where ŌĆśthe Blues’ (Blue Cross and Blue Shield) are the dominant players. … A lot of plans are showing interest, and they’re competing hard.”
He also said smaller insurers were likely to enter various state exchanges.
“This is an attractive market with a lot of covered lives, and smaller companies will probably come in and compete for them,” Holahan said. “Anyone can come into a market, but can you negotiate a good rate with enough (health) providers to keep your premiums down?”
UnitedHealthcare and Cigna, whose primary businesses are the larger group market, are reluctant to jump in too quickly.
“As we have stated publicly for some time, we continue to evaluate exchanges and see 2014 as just the very start of the exchange markets,” Kevin Shermach, a UnitedHealthcare spokesman, said in a statement.
“We will continue ongoing discussions with our provider partners and customers to continually review future exchange opportunities. As the economics, sustainability and dynamics of the exchange continue to become clearer over time, the exchange has the potential to be a growth market with much to offer UnitedHealthcare, other insurers and consumers.”
Anthem Blue Cross and Blue Shield, with an estimated 26 percent market share combined in Missouri’s individual and group markets, sounds more eager.
“As a market place leader in the individual and small employer markets, Anthem is uniquely positioned to succeed in the health benefits exchanges,” Deb Wiethop, an Anthem spokeswoman in St. Louis, said in a statement. “Anthem is actively creating product solutions for the exchange marketplace. … As the health care marketplace shifts to become more consumer and retail focused, we are changing to better meet those needs.”
Assurant Health, a leader in the individual and small employer group market, “plans to participate in exchanges in 2015,” spokeswoman Sue Pierman said.
Humana, based in Louisville, Ky., has announced plans to enter 14 different exchanges across the country in 2014 but has not yet identified those states, its spokesman Jim Turner said. Humana writes only a limited number of individual health policies in Missouri.
Other leading health insurers ŌĆö Aetna and its subsidiary, Coventry Health Care Inc., as well as Clayton-based Centene Corp. ŌĆö may also be planning to participate in the Missouri exchange, according to industry sources. Officials at Aetna, Coventry and Centene did not return phone calls Monday.
“There’s a lot of reluctance to talk about the exchanges, just because there are too many ŌĆśwhat ifs,’ŌĆē” said Cigna spokesman Joe Mondy. “The insurance industry is one of those industries that doesn’t like a lot of what ifs.”
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/big-insurers-opt-out-of-missouri-exchange/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26661&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from our partner the
Dr. Angela Patterson often sees her patients when she eats lunch at Mel’s Diner, an oasis in Puxico, a farming town in Stoddard County in southeast Missouri.
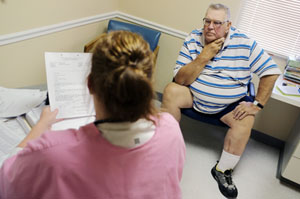
Dr. Angela Patterson talks with patient Jack Miller at Puxico Medical Clinic (Photo by Erik M. Lunsford/St. Louis Post-Dispatch).
Patterson runs a family clinic in Puxico, population 861, where a small staff of physicians and nurses tend to patients who might otherwise not receive care. Their busy offices, located in the rear of a bank building, are cluttered with medical files, a refrigerator for lab tests, an X-ray machine, and supplies.
“I’ve been to patients’ homes. I’ve been to their Little League games. I know who’s getting married and divorced,” said Patterson, a specialist in internal medicine, who grew up in the nearby town of Fisk in Butler County. Her father farmed; her mother taught school.
“We have people here who financially and physically can’t get to Poplar Bluff,” she said, adding that a round-trip drive takes an hour out of your day.
Poplar Bluff Regional Medical Center operates seven family clinics in four rural counties to fill the gap for rural patients, many of whom are elderly and afflicted with multiple chronic conditions such as obesity, diabetes and heart failure. Nearly 60 percent of the clinic’s patients are on Medicare, and some are on Medicaid as well.
“I struggle with being overweight, so I talk with patients about exercise and making changes,” said Patterson, who sees on average 25 patients a day. The clinic’s two nurse practitioners, Kimberly Te and Holly Reed, see additional patients; some need urgent care. Reed also makes rounds in a nearby nursing home and residential care facility.
“I never wanted to be a doctor who just hands a patient a scrip,” Patterson said. “People have to wait. I never operate on time. But when they see me, we may talk for an hour. … I do a lot more mental health care than I thought I would.”
The physician tries to talk with smokers once or twice a year. “To be honest, I don’t badger them every single time,” she said. “People have the right to make poor choices. But I do try to counsel them.”
She nudges her most senior patients toward hospice care, rather than additional diagnostic tests and hospitalization toward the end of life ŌĆö encouraging them to value the quality, rather than quantity, of their days.
“We’re doing pretty well here, but nothing’s perfect,” said Patterson, indicating that she’d like to hire dieticians but Medicare won’t pay for them.
Story Components
- Hospital In Rural Missouri Faces Tough Challenges
- Small-Town Clinic Provides Care To A Farming Community’s Poor
Patterson also treats kids, from age 2 and up. About 46 percent of the children in Stoddard County are covered by Medicaid.
Dr. Bijan Bastaninejad, a pediatric hospitalist, spends five days a month at the clinic ŌĆö handling children’s appointments and walk-ins. Some of these kids, too, are obese and diabetic. “It’s hard to make lifestyle choices, especially if your (family’s) financials are not in place and it’s easier to buy fast food,” he said.
Te, the nurse practitioner, summed up the dilemmas of treating the rural poor. “They’re not ignorant people, but they’re not educated,” she said. “You need to explain how smoking complicates the disease process.”
Te said that many patients cannot afford to buy medicine . “Older people on fixed incomes can’t afford a $25 a month co-pay for a drug when they’re taking eight or 10 pills,” she said.
Ginger Holloway, the clinic’s office manager, said that she often spends 30 or 40 minutes on the phone trying to obtain an insurer’s “pre-authorization” for treatment.
“Insurance pays less and less all the time,” she said. “We have some really sick people who still make too much money to get (government) assistance.”
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/puxico-clinic-rural-health/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26513&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story comes from our partner the
A 30-second television ad shows off Poplar Bluff’s sparkling new medical center as a narrator says, “Welcome ŌĆ” to the future of health care.”

Poplar Bluff Regional Medical Center serves residents of rural southeast Missouri (Photo by Erik M. Lunsford/St. Louis Post-Dispatch)
Robotic surgery systems. High-tech diagnostic equipment. State-of-the-art birthing suites. Poplar Bluff Regional Medical Center, which opened earlier this year, was built at a cost of $173 million by its parent, for-profit Health Management Associates Inc. of Naples, Fla.
But this jewel of a hospital on the edge of a faded factory town of 17,023 residents is only one link in the health care chain’s efforts to serve the region’s rural population. The hospital also operates seven family clinics in four counties of southeast Missouri.
The Affordable Care Act’s success or failure will depend in large part on the efforts of rural hospitals such as Poplar Bluff to treat the poor. It may be in a shiny new building, but it has a long way to go to provide efficient, low-cost medical care in its market. And like other rural hospitals, Poplar Bluff has special challenges.
According to state and regional studies, residents of southeast Missouri face huge obstacles, including some of the state’s highest rates of obesity, diabetes, heart failure and smoking. Many residents have multiple chronic conditions.
Health officials categorize the city of Poplar Bluff and its environs as a medically underserved and high-poverty area with a high proportion of unemployed and uninsured patients. The hospital is considered the remote region’s “sole provider” for certain medical services.
But treating this population isn’t getting any easier. About 70 percent of Poplar Bluff’s patients are Medicare or Medicaid patients, and the number of uninsured and underinsured patients is growing.
The health reform law promised hospitals a windfall of expanded Medicaid coverage, but that has proven to be illusive. Missouri and half the other states have so far balked at broadening their Medicaid programs, resulting in more sick people in hospital emergency rooms without the means to pay.
Story Components
- Hospital In Rural Missouri Faces Tough Challenges
- Small-Town Clinic Provides Care To A Farming Community’s Poor
Poplar Bluff Regional Medical Center has annual revenue exceeding $720 million and a net income of about $24 million, according to the American Hospital Directory. But the hospital’s charity care and bad debt also have climbed significantly in recent years.
“We’re not your typical rural hospital, because of the breadth of our services, from oncology to cardiac surgery and the 1,300 babies we deliver each year,” said Charles Stewart, the hospital’s chief executive. “Our goal is to offer as wide a range of services that it makes sense for the size population that we have here.”
Poplar Bluff’s new acute care hospital has 250 licensed beds, but its top floor is not yet occupied. The hospital delivers more babies than its two nonprofit rivals in Cape Girardeau: Southeast Hospital and St. Francis Medical Center.
Poplar Bluff has three interventional cardiologists and between 35 and 40 additional specialists. It recently began a bariatric surgery program. And hospital executives hope to hire a neurologist and open a neonatal intensive care unit.
“It’s a good hospital,” Ronald Bilbrey, of Poplar Bluff, said recently. “I was out there last night at the emergency department and I got in and out in 20 minutes. At the old hospital, sometimes you’d have to wait four or five hours.”
But some residents still need to be won over by the new facility, which was built to replace Health Management Associates’ dilapidated, crowded hospital across town.
According to the “Hospital Compare” website sponsored by the federal Centers for Medicare & Medicaid Services, only 38 percent of Poplar Bluff’s patients said they would “definitely recommend” the predecessor hospital ŌĆö even though the Joint Commission rated the hospital in 2010 and 2011 as among the “top performers on key quality measures.” That survey was taken before the new hospital opened in late January.
Similarly, the Joint Commission ŌĆö which inspects and accredits hospitals ŌĆö published the results of a 2011-2012 patient survey for the Poplar Bluff hospital which indicated problems in communication, cleanliness and pain management. Only 37 percent of its patients said they would “definitely recommend” the hospital ŌĆö compared to a state average of 69 percent and a national average of 70 percent.
Some local residents, when they or their loved ones need surgery, have grown into the habit of making the hourlong drive to Cape Girardeau.
“A pig’s a pig, no matter what kind of face you put on it,” said Debbie Sliger, a co-owner of Myrtle’s Place, a busy diner in downtown Poplar Bluff. “We used to have two good hospitals here ŌĆö with competition.”
AMENITIES, HIGH COSTS
Poplar Bluff’s new seven-story hospital is a refuge of sorts in a town that has been pummeled repeatedly by factory closings and layoffs. It has all private rooms with views of nearby tree lines and plenty of elbow room at nurses’ stations. What’s more, the hospital’s front lobby boasts the town’s only Starbucks coffee shop.
“The views are soothing. It’s very therapeutic, and it’s unique. ŌĆ” It’s very calming,” said Melissa Samuelson, the hospital’s chief nursing executive. The hospital is close to Mark Twain National Forest and not far from the Ozarks’ lakes and rivers.
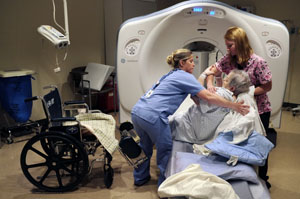
Technicians Misty Lowery and Heather Barker assist patient Pauline Tutterrow to her wheelchair following a CT scan at Poplar Bluff Regional Medical Center (Photo by Erik M. Lunsford/St. Louis Post-Dispatch).
The hospital is accredited to deal with chest pain cases, and working toward certification as a stroke center and, eventually, as a certified trauma center. A helicopter pad can be used to transport severely injured patients to other hospitals.
A hybrid operating room can morph from cardiac catheterization to open-heart surgery, depending on a patient’s needs. The hospital’s top-shelf technology includes two da Vinci robotic surgery systems and one of the state’s few MAKOplasty systems for partial knee replacement and full hip replacements. Robotic devices make smaller incisions, usually resulting in less healing time.
But such amenities aren’t cheap. Similar to other rural hospitals, Poplar Bluff has some of the highest medical charges in Missouri for various common procedures.
Poplar Bluff’s average charges for cardiovascular surgery are $159,957, compared to $94,118 at Mercy Hospital St. Louis, according to the American Hospital Directory. Poplar Bluff’s average charges for orthopedic surgery are $70,495, compared to $46,900 at Mercy St. Louis; its average charges for vascular surgery are $96,912, compared to $55,671 at Mercy; and its average charges for surgery are $130,404, compared to $106,506 at Mercy.
And╠², the Poplar Bluff hospital’s charges for heart attack care, pacemaker implants and fractures of the hip and pelvis are among the highest in Missouri.
When asked about the hospital’s pricing, Stewart said that its rates are discounted heavily for those who cannot afford to pay. He also said that a major factor in the hospital’s pricing is high labor costs, especially the difficulty of recruiting high-end specialists as well as primary care physicians.
“We still have to pay salaries that are competitive with urban centers,” he said, noting that some physicians feel they are making sacrifices by living and working far from a city.
“Sometimes we have to offer quite an extensive package to get a physician to consider coming to Poplar Bluff, Missouri,” Stewart said. “It takes a special physician who wants to come to a rural area and make a difference. We have one of the sickest populations in the state when it comes to obesity, diabetes and heart conditions. ŌĆ” It takes someone who wants to make things better.”
THE IMPACT╠²OF HEALTH REFORM
The Affordable Care Act is pressing rural hospitals to focus on efficiency, convert to electronic health records, and collaborate with more specialized institutions to increase quality of care.
Quality of Care
- The Joint Commission, which inspects and accredits hospitals, lists Poplar Bluff Regional Medical Center as “above the target range value” ŌĆö statewide and nationally ŌĆö for treatment of key conditions, including heart attack, heart failure and pneumonia; infection prevention; and four specific procedures, namely blood vessel surgery, coronary artery bypass, hysterectomy, and knee replacement. The hospital is rated as “similar to the target range value” for hip joint replacement and colon/large intestine surgery.
- The Hospital Compare website, sponsored by the federal Centers for Medicare & Medicaid Services, gives the hospital generally positive marks but lists its death rate for heart failure and pneumonia patients as “worse than U.S. national rate.” Hospital Compare also indicates that Poplar Bluff relies more than leading hospitals on medical imaging, including CT scans and follow-up mammograms, which can increase patients’ exposure to radiation.
Poplar Bluff has received positive reviews from the Joint Commission for its quality of services, including its heart attack and pneumonia care. But the federal Hospital Compare website points out areas for improvement, including that its death rate for heart failure and pneumonia patients is worse than the national benchmark.
To improve its care, the hospital is using “telemedicine” to hook up with neurologists at Barnes-Jewish Hospital in St. Louis to diagnose and treat high-risk pregnancies. Poplar Bluff will soon finish converting its old medical file system to electronic health records that can be easily accessed by doctors and nurses. Federal regulators also will have access to such data and make comparisons between health providers to further assess efficiency and quality of care ŌĆö and penalize hospitals that fail to meet industry norms.
Still, the Poplar Bluff hospital is being squeezed by the private market. Insurers have pressed it and other hospitals to cap or lower their charges. Employer health plans are increasingly requiring that employees pay high deductibles, which results in people putting off elective procedures and diagnostic tests due to the high cost of care.
“Our whole model in health care is changing ŌĆö going from volume-based to quality-based,” Stewart said. “We’re moving into uncharted territory, and it’s becoming tougher for independent hospitals to survive.”
Poplar Bluff’s parent, Health Management Associates, operates 70 hospitals nationwide ŌĆö and presumably has the chops to decipher a changing regulatory scheme and the muscle to exploit economies of scale and negotiate lower rates in buying hospital equipment, medical supplies and pharmaceuticals.
But the Affordable Care Act, with its goal of better medicine for less money, is also nudging hospitals to take greater responsibility and economic accountability for the health of populations they serve. For a rural hospital, that can be doubly difficult.
Stewart said that a first step is education: People need to understand how lifestyle choices and preventive care can affect long-term health. But reaching a rural population is not easy. Poplar Bluff does not have a local TV station nor a single cable network that serves nearby communities. Many residents don’t read a daily newspaper.
There’s also force of habit for a region known for its independent-mindedness.
“We’re talking about a huge cultural change,” Stewart said. “It’s not as simple as telling someone you shouldn’t smoke. It’s going to take incentives by the payers like Medicare and the Medicaid and the insurers to stimulate change. … It’s going to take getting out and trying to make the human connections. It may not be as flashy (as TV, radio, billboards, direct mail and newspapers), but it has a longer-lasting impact.”
If the Legislature expands Medicaid, federal health officials will send billions of dollars to Missouri to help cover medical costs of the poor. But that could simply mean shifting some Medicare dollars to the Medicaid program.
If Medicaid is not expanded, charity care and bad debt will continue to proliferate. Poplar Bluff and other hospitals will need to find new ways to triage their services for the poor and uninsured. To bridge that gap, hospital charges would surely increase for self-pay patients, and individuals covered by an employer’s health plan would need to chip in higher insurance premiums.
“We’re going to be taking care of more people with fewer resources,” Stewart said.
┬ķČ╣┼«ė┼ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at ┬ķČ╣┼«ė┼ŌĆöan independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/popluar-bluff-rural-missouri-hospital-health-reform/">article</a> first appeared on <a target="_blank" href="">┬ķČ╣┼«ė┼ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26523&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>