Only 55,000 of an estimated 151,000 people who applied for the program by Jan. 1 have been enrolled in Medicaid expansion, said Kait Gillis, spokeswoman for the state Department of Human Services.
She acknowledged the delays and said the agency was working to fix them.

For example, advocates say that people with active addictions and mental health issues have been moved from the general assistance program and switched to a private insurer that wasn’t expecting or prepared for their needs.
“There is a level of chaos out there,” said Estelle Richman, head of a special transition team focused on the Department of Human Services for Governor-elect Tom Wolf.
Richman predicted things will “get better quickly” after Wolf takes over Jan. 20. The administration will begin “un-complicating” the system and transitioning it to a full Medicaid expansion.
“This governor campaigned on this issue,” Richman said. “He will make this happen. And he will try to make this happen as quickly as possible.”
An estimated 600,000 Pennsylvanians are eligible for coverage under the Medicaid expansion plan. Medicaid enrollment never closes but open enrollment for individual policies in the ACA marketplace ends Feb. 15.
Healthy Pennsylvania was the signature plan of outgoing Republican Gov. Tom Corbett. His administration got the green light to start the program from the Obama administration in August 2014. Under the program, people in the expansion are getting less coverage than current recipients. And the Corbett administration had also been in talks with federal officials about reducing benefits for those traditional Medicaid recipients.
The chaos and the logjam of applicants waiting for approval are partly due to the Department of Human Services asking people to supply detailed personal financial information – bank account statements, life insurance statements, vehicle value, and retirement account statement – that is not required under Medicaid expansion.
For example, the letter from the state requesting the financial information also says that supplying the information is optional, said Kyle Rouse, a navigator with the Health Federation of Philadelphia.
Rouse said a client brought the letter to him because she was confused. “It confused me as much as it confused her, because in the same letter it said the information was optional but they were requesting it,” he said.
What Rouse and other navigators and advocates have learned is that if their clients don’t supply that information, their application gets stalled or denied.
“The value of your bank account is irrelevant to your eligibility under the extension category,” said Kyle Fisher, a staff attorney for the Pennsylvania Health Law Project. “But practically to get an eligibility decision as soon as possible, I would suggest that you have that information.”
In an email, Gillis, the DHS press secretary, said financial information is required “to determine the eligibility for certain categories” of Medicaid, such as permanent disability. But Gillis agreed that people have been rejected for not supplying financial information “even though it was not required.”
“The department is aware of the issue and is currently identifying who may have been impacted and will continue to work to resolve the matter,” she wrote.
At a press conference held in Philadelphia City Council chambers Thursday, state Sen. Vincent Hughes, D-Philadelphia, said Healthy Pennsylvania was a program “fraught with glitches,” and had caused thousands of Philadelphians to lose their insurance coverage. He and other called on the new governor to act quickly to change the program to a more traditional expansion.
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/applying-for-pa-medicaid-expansion-wait-in-line/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=516041&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This KHN story also ran in . It can be republished for free. (details
Six months into the Affordable Care Act, local mental-health and substance-abuse professionals have yet to see an uptick in clients using their new benefits.
The seeming lack of interest has been disappointing for caregivers, but is not completely unexpected.
“It’s very early,” said Patricia Kleven, director of outpatient mental health services at the Belmont Center for Comprehensive Treatment. “I don’t know what it will look like in six months or a year. But at the moment, not so much.”
Behavioral-health coverage has long been stingier than benefits for medical services. That is especially true for substance abuse.
But the ACA aims to change that by including behavioral health as one of 10 essential benefits that plans must cover in order to be sold on the ACA marketplaces.
So why aren’t people flocking to therapists? People are still learning how to use their new plans. And “there is still a lot of stigma” attached to mental illness, Kleven said.
Caregivers say the main reason people aren’t clamoring for care is Pennsylvania’s reluctance to expand Medicaid, leaving a gap where no subsidized or free insurance is available.
“The main issue is the Medicaid gap,” said Joseph Rogers, chief advocacy officer for the Mental Health Association of Southeastern Pennsylvania. “If you don’t have private insurance and you are not poor enough to be on Medicaid, it is very difficult to get behavioral-health services because not enough people provide it on a sliding-scale basis.”
Rogers said many people that his group helps have serious challenges, from schizophrenia to major depression. Though some work part-time, most can’t hold a full-time job. So they can’t get covered at work and don’t earn enough to qualify for a tax-credit subsidy in the marketplace.
“We know that there are people falling through the [Medicaid] hole,” Rogers said. “If you have private insurance and have enough to pay some co-pay, you are probably going to be able to see somebody. But those people who don’t have money are not going to get the care, and that is disappointing.”
Seeing a therapist regularly can be costly. If one even takes insurance, co-payments can be $25 to $45 a visit. With sessions scheduled weekly, that adds up quickly.
“It does kind of become a trade-off,” Rogers said. “Do I pay the electric bill or do I get some counseling?”
No one expected the health law to fully solve the behavioral-health or substance-abuse problem. Including them as essential coverage, however, has helped focus attention, says Sanjay Nath, director of the Institute for Graduate Clinical Psychology at Widener University.
“For Health and Human Services and the president to put their weight behind the epidemic of substance abuse and have it listed together with mental health is a major shift in policy,” Nath said. “One of the areas the ACA is going to change the most is substance abuse.”
In the past, Nath said, many substance-abuse services – rehabilitation, detoxification, and residential/transitional care – were “carved out” and had stricter rules for use.
Though the ACA makes coverage of substance-abuse treatment essential, it does allow states to choose what insurance will cover, Nath said. Pennsylvania has adopted substance-abuse coverage for in-patient and residential care. And Nath said there were signs other states would follow suit.
The ACA also reinforces earlier laws requiring behavioral-health services to have similar payment rates as medical and surgical practices. Nath hopes that in five years, both fields will be on par.
“If you go back a decade,” he said, behavioral health “had separate co-pays, separate policies, separate contract for behavioral health with worse coverage typically than physical health care. That era is over, and that is a huge relief.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/mental-health/aca-hasnt-boosted-use-of-mental-health-care-services-in-philly-region/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33378&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Success is good. But too much success can leave some people grumbling.Â
Take Independence Blue Cross. The region’s largest health insurer anticipated enrolling 100,000 new members in Pennsylvania and through AmeriHealth New Jersey when the Affordable Care Act marketplace opened in October.Â
As of April 30, the company had signed up a total of 283,000 members in new plans, almost three times as many as it expected. And 89 percent of them have paid their premiums.Â
Great news, right? Well, sure, unless you are among the many people who have telephoned the company and been stranded on indefinite hold with customer service, or been unable to access the company’s website, or who didn’t receive an identification card, or were enrolled in the wrong plan.Â
Success to you probably feels more like incompetence.Â
“We are personally reaching out to our customers and saying, ‘Sorry, here’s what the factors are on hold times,’ ” said Stephan Roker, Independence’s senior vice president of service operations. “All the projections we were given to use we had to amend very quickly.”Â
Underestimating its enrollment caused a domino effect for Independence. Difficulty getting through on the phone led to a 400 percent surge in e-mails that overwhelmed the website, causing a 550 percent increase in Facebook comments complaining about being unable to get through.Â
“Every time we turn a corner, the volume [of new members] increases,” Roker said from Independence’s state-of-the-art call center in Spring Garden. “We’re always busy, but this has been beyond our wildest dreams.”Â
From Jan. 1 through May 2, Independence averaged 25,000 to 30,000 phone calls a day, including a peak of 40,000 calls on one day. That amounted to a 75 percent jump over the same four months of the previous year.Â
During those four months, having someone answer a call took an average of 15 to 20 minutes. Most calls are now answered in five minutes, executives said. There were some cases in those four months, Roker said, in which people were on hold for two hours. That still happens because of the length of the calls, but it’s less frequent, he said.Â
To help ease the backlog, Independence initially increased its phone staff by 20 percent. When that proved insufficient, the company added more people, eventually increasing its customer service staff to 600, a rise of 50 percent.Â
“We do a lot in terms of hiring and looking for people with customer service in their DNA,” said Renee Rhem, Independence vice president of customer service.Â
New hires go through eight weeks of classroom training followed by four weeks of taking live calls under the scrutiny of instructors. Graduates move to the call center, where they become part of a 12- to 15-member team that includes a technical adviser and a team manager.Â
The call center, decorated in soothing tones of blue and gray, stretches across an area the size of one-and-a-half football fields. Customer representatives work in low-walled cubicles designed so they can talk to and learn from one another, and have two computer screens to allow them to access the full spectrum of callers’ information.Â
But it isn’t just the number of calls clogging the phone lines – it’s the length. Calls run on average 25 percent to 30 percent longer than average, Roker said, because many customers are buying insurance for the first time and aren’t familiar with the language. They need to be educated about how things work.
Others are accustomed to having a human resources department handle their health insurance issues. But, mostly, people just want to be sure they have the right coverage.Â
“Health care is very personal,” Roker said. “When you are talking to someone, you are talking about their fears and anxieties. What we are learning is that consumers want to talk to people.”Â
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/insurer-working-hard-to-keep-up-with-call-demand/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33692&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Dean Angstadt fells trees for a living.
He’s a self-employed, self-sufficient logger who has cleared his own path for most of his 57 years, never expecting help from anyone. And even though he’d been uninsured since 2009, he especially wanted nothing to do with the Affordable Care Act.
“I don’t read what the Democrats have to say about it because I think they’re full of it,” he told his friend Bob Leinhauser, who suggested he sign up.
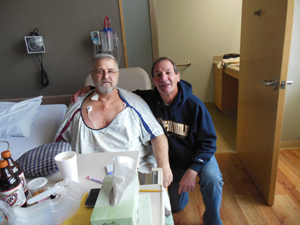
Political odd couple: Dean Angstadt (left) opposed Obamacare until his friend Bob Leinhauser persuaded him to sign up just in time for life-saving heart surgery (Photo courtesy of Bob Leinhauser).
That refrain changed this year when a faulty aortic valve almost felled Angstadt. Suddenly, he was facing a choice: Buy a health plan, through a law he despised, that would pay the lion’s share of the cost of the life-saving surgery – or die. He chose the former.
“A lot of people I talk to are so misinformed about the ACA,” Angstadt said. “I was, before Bob went through all this for me. I would recommend it to anybody and, in fact, have encouraged friends, including the one guy who hauls my logs.”
In 2011, Angstadt had a pacemaker and defibrillator implanted to help his ailing heart pump more efficiently. Not long after, the almost 6-foot, 285-pound man’s man was back in the woods, doing the Paul Bunyan thing.
But last summer, his health worsened again. It was taking him 10 minutes to catch his breath after felling a tree. By fall, he was winded after traveling the 50 feet between his house and truck.
“I knew that I was really sick,” said the Boyertown resident. “I figured the doctors were going to have to operate, so I tried to work as long as I could to save money for the surgery. But it got to the point where I couldn’t work.”
Angstadt called Leinhauser. The political odd couple talked a bit before Angstadt mentioned he was having trouble breathing.
Leinhauser, 55, a retired firefighter and nurse, drove him to a doctor’s office. “Dean only saw a doctor when he needed to because it made a big difference in his finances,” Leinhauser said.
From time to time, Leinhauser would urge Angstadt to buy a plan through the ACA marketplace. And each time, Angstadt refused.
“We argued about it for months,” Angstadt said. “I didn’t trust this Obamacare. One of the big reasons is it sounded too good to be true.”
January came, and Angstadt’s health continued to decline. His doctor made it clear he urgently needed valve-replacement surgery. Leinhauser had seen enough and insisted his friend get insured.
“The only thing he was ever really adamant about was that Obamacare was the real deal,” Angstadt said. “I trusted him to at least take a look at it.”
Leinhauser went to Angstadt’s house, and in less than an hour, the duo had done the application. A day later, Angstadt signed up for the Highmark Blue Cross silver PPO plan and paid his first monthly premium: $26.11.
“All of a sudden, I’m getting notification from Highmark, and I got my card, and it was actually all legitimate,” he said. “I could have done backflips if I was in better shape.”
Angstadt’s plan kicked in on March 1. It was just in time. Surgery couldn’t be put off any longer. On March 31, Angstadt had life-saving valve-replacement surgery.
“I probably would have ended up falling over dead” without the surgery, Angstadt said. “Not only did it save my life, it’s going to give me a better quality of life.”
Angstadt faces a long recovery, but his conversion to ACA supporter is done. The political storm around the ACA, he said, is the political parties “fighting each other over things that can benefit people.”
“For me, this isn’t about politics,” he added. “I’m trying to help other people who are like me, stubborn and bullheaded, who refused to even look. From my own experience, the ACA is everything it’s supposed to be and, in fact, better than it’s made out to be.”
He has also thanked his good friend, Leinhauser, for caring enough to persuade him to buy insurance and have the surgery.
“He has thanked me a couple times,” Leinhauser said. “I just wish he would reciprocate by eating his green beans.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/news/philadelphia-inquirer-health-law-convert/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32813&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Michelle Lamb recalls it being “pretty easy” buying health insurance on the Affordable Care Act marketplace last December.
But using her Independence Blue Cross plan has been maddening.
The 39-year-old West Oak Lane day care teacher has made three monthly premium payments at more than three times her subsidized rate just to make sure she was covered. That’s a steep price for insurance that has been canceled three times – for nonpayment.
“I paid my first premium payment in January and have not received a statement since,” she said.
Lamb’s case may be an outlier. But some people are still getting lost in the download between the government and the insurer.
“In this kind of new market, it’s pretty complex,” said Brian Lobley, Independence’s senior vice president of marketing and consumer business.
Lamb left the site thinking she had insurance for herself and her daughter. Her subsidy cut the $90.70 monthly premium for the Keystone HMO Proactive plan to $25. The ACA customer rep told her the insurer would send her an invoice.
Sure enough, Lamb got a bill in January with a premium of $90.70, the pre-subsidy amount. Worried about being uninsured – or worse yet, about mucking up the system – Lamb paid the full freight and hoped to get the premium figured out later.
She didn’t receive a February invoice. But later that month when Lamb went to pick up a prescription, the pharmacy said it had no record of her plan. Even if Lamb did not pay her February premium, the law states that after making an initial premium payment, an individual’s policy cannot be canceled until two more consecutive payments are missed.
After being on hold for two hours on Independence’s customer service line, she went to its Market Street headquarters. A rep there confirmed that her account had been suspended for nonpayment.
“She couldn’t tell me why there was a hold on my account,” Lamb said. “But she said I should make a payment because it could happen again.”
Lamb plunked down another $90.70 on the spot.
March roared in sans invoice. Concerned, Lamb called Independence to ascertain that her account was fine and that she was covered. It wasn’t. She wasn’t. Her policy had again been canceled, even though she had paid – in person – a few weeks earlier.
That payment, the phone rep said, covered February’s premium. But under the two-consecutive-missed-payments rule, Lamb’s policy should still have been active. “So I made another $90.70 payment over the phone,” she said. “That’s where I’m at. I haven’t paid anything for April.”
Since she complained to The Inquirer, Lamb said, the insurer has promised to “straighten everything out. I’m pleased with the conversation but nothing has been done yet.”
Though privacy laws forbid Lobley from discussing members, he said cases like Lamb’s were rare. Those that do occur often are traced to communication mix-ups between the marketplace and insurer.
Only the government can set an individual’s subsidy, he said.
The insurer keeps wrestling with other issues like members’ multiple enrollments. Some need “hand-to-hand research.”
“We have to fix our model in how we respond to customers,” he said. “We want to make sure we’re using situations, as lessons learned, to improve.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/philly-fully-paid/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=33022&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership withÂ
There were plenty of nights during the last 33 years that Denise Schroeder of West Chester had to choose between eating dinner and paying for health insurance. And no, that is not an exaggeration.
Schroeder is a cancer survivor, and for many of those years, a working, single mom who felt lucky just to have coverage. Schroeder, who owns Happy Heart Clown ‘N Stuff, a party entertainment firm, always fed her daughter but skipped meals herself when money was tight to ensure she could pay the $700 monthly premium.
With her savings account long since drained, her retirement fund exhausted, and an $880 monthly premium payment gobbling up almost half of her annual income, Schroeder, 62, could no longer make financial ends meet.
Then she heard about the Affordable Care Act. “I thought maybe this was my saving grace,” Schroeder said.
Schroeder bought Independence Blue Cross’ silver Keystone HMO. When the navigator said that her new premium payment was $22 a month – $858 less than she paid last month – Schroeder burst into tears.
“I have to know exactly what is covered and what isn’t, and which doctors and specialists are on the list for this policy,” she said. “It was nice paying the premium and then buying a few groceries.”
Even as people continue enrolling to buy insurance plans through mid-April, Independence is focusing on the next phase: Helping people like Schroeder learn how to use their new ACA policies.
“We are fully aware that the process doesn’t stop with the sale,” said Paula Sunshine, IBC’s vice president for consumer products. “We have a well-developed on-boarding program.”
That program may have to expand since the company enormously underestimated its number of new enrollees. How enormously? Let’s just say Independence might want to consider hiring statistician extraordinaire Nate Silver to make its next projection.
More than 110,000 people in the Philadelphia region and 68,000 consumers in New Jersey, through its AmeriHealth subsidiary, signed up for Independence plans, the insurer said. That was roughly 50 percent more than the company predicted and a five percent bump in overall membership.
“We’ve been blown away by the overall enrollment,” said Dan Hilferty, Independence’s president and CEO.
Those numbers are more impressive when compared with the reported 75,000 to 100,000 people enrolled nationally by insurance giant Cigna. And Independence’s social-media efforts also seems to have paid off. The highly sought-after, young “invincibles” – 18-to-34-year-olds – were 27 percent of new enrollees. Customers 35 to 44 accounted for 15 percent, while those 45 and above totaled 21 percent.
“Now we have to service them,” Hilferty said. “We’re trying to be proactive.”
The company is contacting new members via regular mail, e-mail, and phone to help them get up to speed, Sunshine said. New members will be asked if they have received an identification card, if they understand their plan’s benefits, and, yes, if they have made their premium payment.
Sunshine said special attention will be given to people who bought Independence’s best-selling silver HMO Keystone Proactive tier plan. New to the market, the plan has three tiers. Policy holders with a referral can use doctors and hospitals at any tier level. But deductibles, co-payments and coinsurances can vary dramatically.
To reach its Proactive enrollees, Independence is analyzing data on where people live so it can dispatch its Independence Express to hold neighborhood seminars. The goal is to make sure people understand the tier system – how one hospital could cost members three times more than another – and how the drug formulary works.
“We want to educate the public on how to use their benefits,” Sunshine said. Members can call the company’s customer service line at 888-879-4891.
Both Sunshine and Hilferty acknowledge that the company’s call center has at times left people on hold for hours.
“We need to apologize,” Sunshine said. “That is not the way we want to do business. We need to be better at it and we are putting every effort behind that.”
Schroeder is excited about going to a meeting to learn more about her plan’s benefits. “If it is in my area or close by, I will definitely go,” she said. “Knowledge is power, and I’m going to utilize the system as much as I can.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/philadelphia-inquirer-boost-from-health-law-for-clients-insurers/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32854&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with ![]()
It’s a job where stress mounts like dollars on a taxicab meter. The hours are long, the wages are low, and the competition for customers is often fierce.

Rodrigo Giraldo (left) helps taxi driver Jimmy Solomon apply for health insurance. (Michael S. Wirtz/The Inquirer)
Toss in an eat-on-the-go, fast-food diet, little exercise, a sore back and achy joints from jockeying through traffic all day and you start to grasp the burdens Philadelphia cabdrivers face.
“It’s a high-stress job,” said Ronald Blount, president of the Unified Taxi Workers Alliance of Pennsylvania, which represents 1,200 of the city’s 5,000 cabdrivers.
Blount said drivers suffer from maladies like high blood pressure, , and heart and stomach issues. Their ailments almost always go untreated because cabbies are considered independent contractors responsible for their own .
Until recently, the price of an individual plan was unaffordable for most Philadelphia hacks, who make $350 to $400 per 70-hour work week. But now the union, with help from Enroll America and Healthy Philadelphia, is heading a drive to get the city’s cabbies signed up via the Affordable Care Act marketplace.
“We felt this was a perfect opportunity for drivers,” said Blount, 54, who has been carting people around the city since 1980. “For a lot of drivers, this is the first time they will have health insurance.”
Since starting its push in December, the union has signed up 750 cabdrivers. It has also begun helping cabdriver groups in other cities replicate its success.
“No other taxi organization is doing this kind of work,” said Mohammad Shukur, the union’s senior vice president.
Getting the campaign off the ground is hard work. Blount wants all drivers, not just union members, to know that affordable insurance is available. So the union uses word of mouth and text messages sent by the Philadelphia Parking Authority’s GPS system to in-cab monitors to alert drivers when navigators are available at the union office in an old church at 4221 Chestnut St.
“I tell drivers to come here because we do a very good job,” said Shukur, of Upper Darby, who has been driving for 12 years. “There is a huge demand.”
Some of the drivers who went to the early sessions had tried but failed to sign up on their own. They needed help from navigators to buy a plan. But most taxi drivers know little about the ACA.
“A lot of drivers were not computer-literate,” Blount said. “Even the basic stuff. They needed an e-mail address, and we had to walk them through the application.”
Then there is the language issue. The union represents drivers from more than 40 nations. That means dealing with 40 languages, customs, cultures, and religions.
“We always have people here who can speak the languages,” said Shukur, 45. “We have navigators on each of the computers and they sit down and help. Within 35 minutes, they are finished.”
Drivers who complete the application but don’t buy a plan are asked to write their name and phone number on an Enroll America postcard. A worker then follows up to make sure the drivers get covered.
“People are very happy with the insurance they receive,” Shukur said.
Blount estimated 80 percent of the drivers the union had enrolled qualified for a subsidy. Some drivers are paying a premium of just 14 cents a month; others have locked up policies for $35 to $70 a month. Blount said they caution every driver not to choose a policy based solely on the monthly premium but to look at such factors as doctor and hospital networks, drug costs, and deductibles.
“We tell them that they have to look at the whole picture,” said Blount, who lives in North Philadelphia. “What we are trying to do is steer them to the preferred provider organization plans that give them more options.”
Blount said the union would host sessions every Wednesday, Thursday, and Friday until open enrollment ends on March 31. He wants every driver to be able to get a yearly checkup.
“We are trying our best to enroll all of them. This is a great opportunity.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/union-pushes-to-get-philadelphia-cab-drivers-insured/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=32741&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
As the Affordable Care Act wobbles into its second month, more people are enrolling on the healthcare.gov website and learning if they are eligible to get a subsidy and what their monthly premium payment could be.
Not everyone is happy, especially those who happen to be just above the subsidy cutoff.
Some single older adults who don’t qualify for a subsidy – the cutoff is $45,980 for one person – are pulling out dictionaries (it’s a book older people use) and rereading the definition of affordable.
In Southeastern Pennsylvania a silver-tier plan, which covers 70 percent of insurance costs, can carry a monthly premium of $575 to $1,012, depending on the plan.
For middle class married couples who don’t have children, the subsidy cutoff is $62,000. A silver-tier policy premium for two can range from $1,150 a month to $2,021, again depending on the plan.
Some of those couples are complaining that the law has a hidden marriage penalty. Here’s why: Say a couple has a household income of $70,000 with one spouse making $30,000 and the other $40,000. Combined, they are ineligible for a subsidy. But if they were just living together, each would be eligible for a subsidy.
“We’ve known all along that some people will do better in this market and some people will do worse,” said Joel Ario, a managing director at Manatt Health Care Solutions and a former Pennsylvania insurance commissioner. “In the long run everyone gets more stability out of the marketplace.”
The ACA, like the tax code, is complicated, and it sometimes provides a marriage subsidy and a penalty, said Mark Duggan, a health economist at the University of Pennsylvania’s Wharton School.
“Will it encourage some weird stuff like some people getting divorced? Yeah,” Duggan said. “That was the challenge of this thing. Where do you draw the line?”
The line was drawn using the 2012 federal poverty level. People with an income between 100 percent and 400 percent of that number are eligible for subsidies when they buy health insurance in the ACA marketplace. That amounts to 64 percent of Americans, said Duggan.
“That is a pretty big chunk of the population that is getting a subsidy,” he said. “They could have extended the subsidy to 74 percent of the people under 500 percent of the poverty line. But that would have cost more.”
One fact that has been lost amid the bumbling of the law’s rollout is that health costs are now rising at the slowest pace in 50 years.
“So overall we are bending the price curve better than we have in 50 years,” Ario said. “We can argue about whether the ACA has a lot to do with that or only a little. That is disputable. What is not disputable is that in the end, people are getting less health care cost increases year over year than they have gotten in 50 years on average.”
Another thing that is clear is that changing the way health insurance is delivered in America is a huge undertaking. Before that change can be made, people have to realize “that there will be a significant amount of destruction,” Ario said. In other words, the country will have to break a few eggs to make this omelet.
“It is somewhat complicated,” Duggan said. “But the hardest time with something like this is in the beginning. Medicare Part D was a mess, a total mess for the first several months. What matters for half of the population is that they don’t need to know the million different provisions of the law. They need to know how to get coverage.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/insurance/some-face-marriage-penalty-for-subsidies/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=25710&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
Almost two months after its inglorious rollout, the healthcare.gov website appears to be slowly recuperating. But even if it is 80 percent healed by November’s end, as some public statements suggest, it likely won’t be the promised seamless shopping experience where consumers can compare plans and prices and see if they qualify for premium and cost-sharing subsidies.
Several websites have stepped into the breach and are helping consumers unravel the differences among the various health insurance policies.
When it comes to southeastern Pennsylvania, you can find Independence Blue Cross plans and a subsidy calculator at which was built using real, regional market prices.
“If you go to any of the national sites, [the estimate] will be based on the national silver plan cost,” said Paula Sunshine, IBC’s vice president for consumer affairs. “Our calculator uses the second-lowest-priced silver plan in our market area, so it will represent more accurately what you are going to see [at] the federal site.”
Using information such as household income, the number of children, and the number and ages of the adults covered by the plan, the calculator determines subsidy eligibility. Those deemed eligible are given the amount of monthly premium assistance as well as the household’s federal poverty level percentage. Both figures are needed to get the cost-sharing subsidy.
People qualifying for a subsidy must go to the federal marketplace to buy health insurance. Those who aren’t eligible can shop, enroll, and buy a policy right on IBC’s website.
The site is already getting 10,000 hits a month, Sunshine said. IBC’s calculator will also be available soon as a mobile app that will include live-chat and click-to-call options.
“We’re trying to intercept you before you even talk to an agent and put capabilities on your phone at your fingertips, including our subsidy calculator,” Sunshine said.
ValuePenguin.com took flight in June to give health insurance shoppers an idea what plans would look like when the marketplace opened. Extrapolating from the data insurers must file with states, Jonathan Wu and his partners accurately decoded premium costs and constructed exchanges for 10 states. But when Healthcare.gov failed to function adequately on Oct. 1, Wu and his partners expanded their tool nationwide.
“The one universal that we are seeing is that people are really hungry for information,” Wu said, noting that 150,000 people had visited the site. “They want to understand what the prices are and what benefits are and how they should think about health insurance. Our goal is to provide as much of that as possible.”
Wu’s team has been able to accurately calculate subsidy and premium amounts for various age groups, usually to within a dollar. The website also houses benefit information for 70 percent of plans in the marketplace, something Wu said similar calculators don’t have.
“A lot of people find these plan names on Healthcare.gov or some other site that talk about premiums, but they can’t find the benefits,” Wu said. “And that is actually the second part of the equation and, in fact, is more important than just the premiums.”
ValuePenguin.com is an information-only site, but provides links to ehealthinsurance.com and other health insurers for people interested in buying a policy. Wu and company are working on a program to help consumers choose a health insurance plan.
“What we would really like to do is create a framework for how people should think about how the benefits are laid out in particular plans,” Wu said, “and why you may want to chose a platinum plan versus a catastrophic or bronze plan.”
InsuranceQuotes.com, among the newest subsidy calculators, began building its site in the spring. The website, owned by Bankrate.com, went live Nov. 11.
“It’s different from a lot of calculators because we don’t just give you a number,” said Laura Adams, InsuranceQuote.com’s senior insurance analyst. “You see the options and go ahead and get enrolled.”
Like many calculators, InsuranceQuote.com is designed for shopping and as an information source and is not licensed to sell health insurance. A shopper is linked to getinsured.com, a Web broker connected to the federal data hub where the consumer’s income, citizenship, and residency status are verified and the transaction can be completed.
“What we are providing is what we consider a really simple user interface to take people through the process,” Adams said. “This tool not only allows consumers to figure out if they are eligible for a subsidy, but also if they are eligible for other subsidized health options, and then takes them directly to the site where they would actually enroll.” Online Calculators
The health insurance and subsidy calculator websites are:
HealthSherpa
ValuePenguin
InsuranceQuotes.com
Independence Blue Cross
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/health-industry/websites-step-up-to-fill-federal-void/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=26167&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>This story was produced in partnership with
The frosty weeks before the holidays were always the hot season for Andre Butler. He would head downtown, looking snappy in his “blacks and whites” – industry argot for tuxedos – to work as a bartender, server, or host in Center City’s finest hotels.
But post-recession, those parties have become fewer and smaller. The only reminder for Butler of those days is the constant ache in his legs and hips from the years of lugging heavy trays. He needs tests to pinpoint the cause of his pain, but lacks insurance or the money to pay out-of-pocket.
“Right now, I have basically relegated myself to heating pads, Tylenol, and Motrin,” Butler, 48, of Chestnut Hill, said.
Butler, who has never had a job with insurance, was hoping to buy a plan on the Affordable Care Act marketplace. But he earns too little to qualify for the exchange.
Even more frustrating, he makes too much for Medicaid.
And because Pennsylvania has so far declined the federal money to expand Medicaid, Butler will likely enter the new year uninsured.
“When a politician goes to a hotel to have a function, it is the housekeeper, bell captains, the front desk people, the concierge, and the parking valets who they count on to help them,” Butler said. “Like myself, they don’t have health insurance. We need our health insurance.”
As many as 400,000 Pennsylvanians will plunge into the hole between traditional Medicaid and the new marketplace come Jan. 1, according to the Pennsylvania Health Access Network.
“The overwhelming majority of these people are working,” said Athena Smith Ford, the network’s advocacy director. “Seventy-five percent of them have at least one full-time worker in the household. We’re talking about hairdressers, home health aides, auto mechanics, and servers, people who work in low-wage jobs that don’t come with health insurance and who don’t make enough to purchase it in the private insurance market.”
That gap was supposed to be filled with federal money states could use to cover more people. Gov. Corbett first chose to turn down the so-called Medicaid expansion. Officials have since presented a 12-page plan called Healthy Pennsylvania to the federal government. The aim is to reform Medicaid, increase access, and stabilize financing. The feds have yet to render a decision on the plan.
“We continue to meet and talk with the U.S. Department of Health & Human Services about the Governor’s Healthy Pennsylvania plan and specifically, the plan for Medicaid reform,” e-mailed Christine Cronkright, the governor’s deputy communications director. “These discussions are helping to inform our process in drafting a waiver for the Medicaid program that will require approval by the federal government. We are working through that process as quickly as possible and are hopeful on the front end that conversations with the Centers for Medicare & Medicaid Services and our recent submittal of the formal white paper outlining our requests will expedite approval of the waiver.”
Though Ford and other members of the Cover the Commonwealth Campaign view Healthy Pennsylvania as a good first step, they said the Medicaid expansion would save taxpayers up to $1 billion over the next decade.
“There is bipartisan support in the state House and Senate,” she said. And a recent American Cancer Society poll found that most Pennsylvanians agreed accepting the federal money “is the right thing to do.”
Not taking the money to expand Medicaid may also affect the fiscal health of hospitals. Under the old insurance system, hospitals received federal money to help offset the cost of treating uninsured patients. But the health law eliminates a large chunk of that money beginning in 2015.
“Our hospitals are going to lose at least $8.1 billion in the next 10 years in funding to help pay for uncompensated care,” Ford said. “The hospitals were willing to give it up because they said it was actually going to benefit them if the majority of Pennsylvanians have health insurance coverage either through Medicaid, the marketplace, or an employer.”
Â鶹ŮÓĹ Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at Â鶹ŮÓĹ—an independent source of health policy research, polling, and journalism. Learn more about .This <a target="_blank" href="/medicaid/in-pennsylvania-a-big-gap-in-health-insurance-coverage/">article</a> first appeared on <a target="_blank" href="">Â鶹ŮÓĹ Health News</a> and is republished here under a <a target="_blank" href=" Commons Attribution-NonCommercial-NoDerivatives 4.0 International License</a>.<img src="/wp-content/uploads/sites/8/2023/04/kffhealthnews-icon.png?w=150" style="width:1em;height:1em;margin-left:10px;">
<img id="republication-tracker-tool-source" src="/?republication-pixel=true&post=25986&ga4=G-J74WWTKFM0" style="width:1px;height:1px;">]]>